Archive for category: Clinical Care

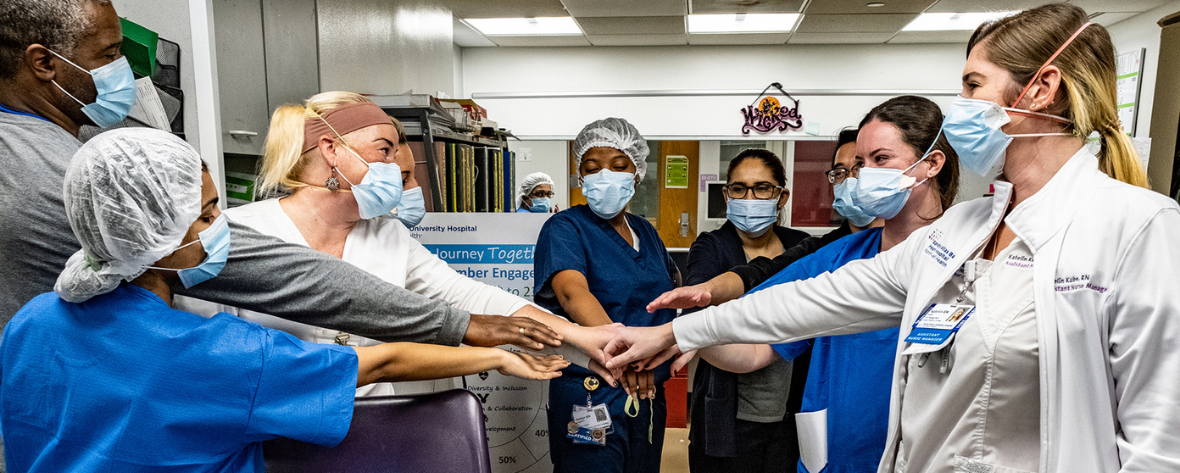
Northwell recognizes two of our extraordinary team members in honor of Autism Acceptance Month
April is National Autism Acceptance Month, and here at Northwell Health, we are dedicated to supporting individuals on the autism spectrum, whether they are members of our staff or the family of our employees.
Our commitment to a diverse workforce that provides a safe and welcoming environment for people with disabilities led to the creation of our N-ABLE BERG (Business Employee Resource Group). The N-ABLE BERG was designed to advocate, educate, and support our employees of all abilities and their families, ensuring everyone has the resources they need and the respect they deserve.
Here, we recognize two of N-ABLE BERG’s members as they share what working at such an inclusive, affirming, and respectful workplace means to them.
Patricia Troiano, Senior Pharmacist at Long Island Jewish Medical Center
Juggling a clinical career while raising a family can be challenging for anyone, but when you are the mother of twin boys on the autism spectrum, finding a supportive work environment is crucial. For 35 years, Patricia Troiano has found that place here at Northwell. As a registered senior pharmacist at Long Island Jewish Medical Center (LIJMC) specializing in sterile compounding and dispensing, Patricia’s role allows her to fulfill prescription orders and provide IV medication to our patients.
A passionate advocate for the autistic population, Patricia says that being part of the N-ABLE BERG this past year and being given the title of Neurodiversity Project Leader in March has given her companionship, comfort, and an opportunity to spread awareness about autism—all crucial to her fulfillment at work and home.
Patricia has also taken advantage of Northwell’s many continuing education offerings, which have enabled her to develop new skills and flourish in her career. Plus, the culture at Northwell has fostered a real family atmosphere—what Patricia says her co-workers call the “pharmily.”
“We really care about each other and are supportive of each other’s lives outside of work,” she says. “My department has been very empathetic during my family’s autism journey by providing support to me as well as the organizations I volunteer for.”
In fact, her department is raising money to purchase a laptop for her son Christopher’s program, The Nicholas Center, which provides vocational and community programs for those with developmental disabilities.
Through good times and bad, her co-workers “kept me going with encouragement and love,” Patricia says. And she’s proud to note that one of her sons on the spectrum is a Northwell employee, making her career well cared for a true family affair.
Tina Chuck, Advisor with Fair Employment Practices
Tina Chuck joined Northwell in 2011, and just three years later, she formed the Office of Research Policy and Training at the Feinstein Institutes, which evaluates and manages centralized policies, research training, and professional development. Shortly thereafter, her young son was diagnosed on the autism spectrum. It was a very stressful time, as she was managing her new job responsibilities as the director, while trying to find the right work-life balance.
“Thankfully, I had supportive colleagues and reported directly to someone who proactively checked-in on my well-being and taught me how to self-advocate,” says Tina. “I am thankful to have the flexibility in my schedule to care for my son and have access to fabulous professional development resources.”
Now Tina will continue her journey this month as Advisor with Fair Employment Practices in which she is excited to get more involved with Northwell’s workforce equity, diversity, and inclusion strategy and focusing on a broad range of initiatives, including helping support and continue to evolve our BERGs and other social belonging and inclusion initiatives. Recently, she became the co-chair of the N-ABLE BERG and through N-ABLE, Tina has been able to apply her skills and work on programming and events focused on enhancing employee and patient experience for those who are neurodiverse. Her professional network grew as each new N-ABLE BERG initiative connected her with people across the organization and within the community and expanded her knowledge and dedication to diversity and inclusion.
“The opportunities are endless at Northwell,” says Tina, citing everything from team-building activities such as cooking at the Ronald McDonald House to making birthday boxes and duffle bags through Together We Rise for children in foster care.
“I love the passion and grit I see in my colleagues, and their selflessness in rolling up their sleeves to step out of their immediate job title to help others.”
Learn more about Northwell’s commitment to diversity and inclusion. Become part of our team by exploring our wide range of career opportunities here.
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Recent Posts
- Explore two different career paths beginning as a nurse extern at Northwell Health.
- Mentorship, desired career growth, and making a difference: Meet Christopher, emergency department registered nurse
- Explore career paths in pharmacy at Northwell Health.
- From quality to operations: Discover Shivani’s career journey in labs
- Discover Tyler’s career journey in facilities and support services at Northwell Health
Categories
- Academia and Research
- Administrative Support
- Advance Clinical Providers
- Business
- Career Advice
- Career Paths
- Clinical Care
- Clinical Laboratory Science
- Clinical Support
- Culinary and Hospitality
- Culture
- EVS
- Featured Articles
- General Management
- Human Resources
- Imaging
- Inclusion and Belonging
- Information Technology
- Mentorship
- Nursing
- Operations
- Patient and Customer Experience
- Pharmacy
- Rehabilitation Services
- Revenue Cycle
- Social Services
- Students and Internships
- Veterans
- Wellness & Benefits
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
Raise your Career Expectations with these Top Reasons to Work Night Shifts at Northwell Health
Working night shifts at Northwell Health comes along with several benefits that can make a positive impact on your overall health and wellbeing. As a Fortune 100 Best Companies to Work For®, Northwell offers career growth opportunities that are easily attainable to night shift professionals in labs and nursing roles. Check out our top reasons below, and jump start your journey to a career well cared for.
Check out our available positions in Labs, Nursing, and Nursing Support.
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Recent Posts
- Explore two different career paths beginning as a nurse extern at Northwell Health.
- Mentorship, desired career growth, and making a difference: Meet Christopher, emergency department registered nurse
- Explore career paths in pharmacy at Northwell Health.
- From quality to operations: Discover Shivani’s career journey in labs
- Discover Tyler’s career journey in facilities and support services at Northwell Health
Categories
- Academia and Research
- Administrative Support
- Advance Clinical Providers
- Business
- Career Advice
- Career Paths
- Clinical Care
- Clinical Laboratory Science
- Clinical Support
- Culinary and Hospitality
- Culture
- EVS
- Featured Articles
- General Management
- Human Resources
- Imaging
- Inclusion and Belonging
- Information Technology
- Mentorship
- Nursing
- Operations
- Patient and Customer Experience
- Pharmacy
- Rehabilitation Services
- Revenue Cycle
- Social Services
- Students and Internships
- Veterans
- Wellness & Benefits

Jennifer Tutone experiences nearly three decades of career growth as a clinician at Northwell
A wise leader once said, when a door opens, don’t be afraid to walk through it. Jennifer Tutone has had many doors open during her 27-year career journey at Northwell Health and she has walked through every one with encouragement from her leaders. Each time, the other side presented opportunity and growth and she continues to embrace new professional experiences at Northwell.
Today, Jennifer is an assistant director of Patient Care Services and Nursing Administration at Staten Island University Hospital with administrative oversight of the hospital inclusive of operational needs, staffing, and patient experience. However, her Northwell career journey began in 1994 as a behavioral health nurse at Zucker Hillside Hospital. During her career journey, she worked across many hospital sites at Northwell and held many roles such as staff nurse, clinical practice coordinator, ambulatory health nurse, assistant director for nursing, site transformation manager, nurse manager, director of information technology, corporate director of innovation, and director of nursing. “Working for Northwell Health has presented me with opportunities to follow my passion for patients and nursing,” says Jennifer.
Jennifer was offered many positions internally because of the skills she learned with each role and her desire to continue learning. There were certain projects she led which opened up doors to new skills and advancement opportunities in roles she never imagined. “What I have learned from each position is to be agile, I have increased my skillset for project management, increased my skillset to being able to acclimate to a role quickly, and I have embraced the organization’s culture to become successful.”
Along her career journey, she had many opportunities to expand her knowledge and grow her skills. Jennifer received tuition reimbursement from Northwell and obtained a Bachelor of Science in Nursing and Master in Public Health. In addition, with the support of her leadership team, Jennifer grew her leadership skills and became responsible for significant projects that impacted the way our organization cares for patients in and out of the hospital. Their encouragement and support created an atmosphere of caring and development which allowed Jennifer to soar to her highest potential. “I am grateful for all of the opportunities which have been presented to me, as they have created the clinician I am today,” Jennifer.
“I value the fact that I can still call Northwell “home” after working here for 27 years and I am incredibly grateful to the individuals I have met along my career journey. My Northwell family will always be special to me and I look forward to continuing to create relationships as my journey within the organization continues.”
Share this entry
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Recent Posts
- Explore two different career paths beginning as a nurse extern at Northwell Health.
- Mentorship, desired career growth, and making a difference: Meet Christopher, emergency department registered nurse
- Explore career paths in pharmacy at Northwell Health.
- From quality to operations: Discover Shivani’s career journey in labs
- Discover Tyler’s career journey in facilities and support services at Northwell Health
Categories
- Academia and Research
- Administrative Support
- Advance Clinical Providers
- Business
- Career Advice
- Career Paths
- Clinical Care
- Clinical Laboratory Science
- Clinical Support
- Culinary and Hospitality
- Culture
- EVS
- Featured Articles
- General Management
- Human Resources
- Imaging
- Inclusion and Belonging
- Information Technology
- Mentorship
- Nursing
- Operations
- Patient and Customer Experience
- Pharmacy
- Rehabilitation Services
- Revenue Cycle
- Social Services
- Students and Internships
- Veterans
- Wellness & Benefits
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019

Attention Biochemistry Majors: Five Great Career Opportunities to Explore at Northwell Health
You either have a degree in biochemistry or are on your way to obtain one — congratulations! Biochemistry requires focus and attention to detail, plus deep knowledge of the chemical processes necessary for life to exist. But there are other career options to explore with this degree plus some additional qualifications and/or certifications. Here are five potential career opportunities at Northwell Health related to this degree. *
Lab Technologist
First, find out more information about your school’s clinical lab science / medical lab tech programs to enroll in this program, which is a requirement, and look to Northwell to start your journey.
When exploring a career as a lab technologist, you’ll learn to set up and perform a variety of routine and/or complex laboratory tests and procedures relevant to the particular lab area and your qualifications. You’ll prepare and test specimens for examination and report results while gaining the skills to perform routine and/or preventive maintenance on laboratory equipment, as well as troubleshoot basic technical problems. Explore positions and qualifications.
Anesthesia Tech
An anesthesia tech assists the anesthesiologist by setting up equipment and preparing various intravenous medications as directed. A big role is testing and maintaining the anesthesia equipment. This includes maintaining supplies and medication inventory, washing, and sterilizing reusable equipment and the anesthetic machine. An anesthesia tech also reports malfunctioning equipment to appropriate personnel. Explore positions and learn more about the requirements for this profession.
Clinical Research Coordinator
Responsible for the coordination of a designated study or group of studies, clinical research coordinators oversee the recruitment of subjects, implementation of study procedures, and collection and processing of data in research projects. For this role, attention to detail is key, as some tasks require keeping accurate and up-to-date records and managing labels, logs and processes. You’ll oversee shipments of biological specimens for analysis according to protocol and training requirements. You’ll get the opportunity to collaborate with physicians, investigators and other healthcare providers when scheduling subjects for protocol-related evaluations. Evaluating results of assessments as related to study protocol comes with the territory and is a major component in this role. In this position, you may have to organize all phases of the grant process, including connecting with funding agencies and build stronger relationships with external partners. Explore opportunities and qualifications for this profession.
Research Technician
Our research technicians collect and process specimens in accordance with established handling protocols. They also administer tests or basic examinations of research subjects. In this position you’ll administer data collection for laboratory equipment and perform initial data analysis and interpretation. You’ll also conduct library research and literature searches using various computer systems, and assist in editing scientific publications, abstracts and posters. Lean more about this profession and review job qualifications.
Clinical Data Analyst
A clinical data analyst analyzes, verifies, tracks and reports on trends data. You’ll gain the experience of maintaining consistency and integrity of data collection and will be expected to report concerns regarding data integrity. You’ll work in collaboration and build connections with various departments across Northwell Health in database development and required modifications. Explore positions and qualifications.
Start Your Job Search With Us!
Discover what Northwell has to offer as you begin your career journey after graduation.
Browse our careers website to learn more about all of Northwell Health’s current open positions and read the job descriptions to identify roles you’re both qualified and interested in.
See anything you like? Apply! Please keep in mind we only except applications through our careers page, and not through email. If you have any questions, contact us at campusrecruitment@northwell.edu.
*Additional degrees/certifications may be required for select roles highlighted above.
To explore more available opportunities at Northwell Health, check our Careers page.
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Recent Posts
- Explore two different career paths beginning as a nurse extern at Northwell Health.
- Mentorship, desired career growth, and making a difference: Meet Christopher, emergency department registered nurse
- Explore career paths in pharmacy at Northwell Health.
- From quality to operations: Discover Shivani’s career journey in labs
- Discover Tyler’s career journey in facilities and support services at Northwell Health
Categories
- Academia and Research
- Administrative Support
- Advance Clinical Providers
- Business
- Career Advice
- Career Paths
- Clinical Care
- Clinical Laboratory Science
- Clinical Support
- Culinary and Hospitality
- Culture
- EVS
- Featured Articles
- General Management
- Human Resources
- Imaging
- Inclusion and Belonging
- Information Technology
- Mentorship
- Nursing
- Operations
- Patient and Customer Experience
- Pharmacy
- Rehabilitation Services
- Revenue Cycle
- Social Services
- Students and Internships
- Veterans
- Wellness & Benefits

Day in the Life: Respiratory Therapist at North Shore University Hospital
Meet Lian Shanhai, who started her Northwell career journey in 2020 as a respiratory therapist with a neonatal/pediatric specialty certification at North Shore University Hospital (NSUH). Within her first year at Northwell, Lian has learned to be a team player and develop skills that helps her grow as a Respiratory Therapist.
Her day-to-day routine varies but her current role includes performing respiratory care as prescribed by a provider for the diagnosis and treatment of respiratory illness in patients of all ages, from premature newborns to geriatric patients. Within her role she responds to all codes, Level I traumas, and rapid responses depending on her assignment for her shift.
First things first, Lian looks to see what her assignment is for the day once she arrives to work. Next, she prints out her patient list, which includes their ordered treatments. Then she reads the report from the previous shift and attends a huddle meeting, after which she goes to her units. This is where her team begins their rounds with the providers and develops a plan for the day, which can include examining patients’ airways and suctioning when necessary, performing ventilator checks, and providing additional treatments. “During the shift I also assist with intubations, transport patients on ventilatory support to procedures and attend high-risk deliveries in Katz Women’s Hospital at NSUH,” says Lian.
“My favorite thing about being a respiratory therapist is the connections I get to make with my patients and their families,” says Lian. “I treat every patient I come into contact with as if they were my own family and I’m able to provide relief for my patients.” Part of Lian’s role is to explain to family members how the ventilator works and how we are helping their loved ones. “It is very difficult to see a loved one intubated and on a ventilator but I get to provide peace of mind to their family members.”
Looking to discover a career well cared for as a respiratory therapist? Apply today!
Share this entry
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Recent Posts
- Explore two different career paths beginning as a nurse extern at Northwell Health.
- Mentorship, desired career growth, and making a difference: Meet Christopher, emergency department registered nurse
- Explore career paths in pharmacy at Northwell Health.
- From quality to operations: Discover Shivani’s career journey in labs
- Discover Tyler’s career journey in facilities and support services at Northwell Health
Categories
- Academia and Research
- Administrative Support
- Advance Clinical Providers
- Business
- Career Advice
- Career Paths
- Clinical Care
- Clinical Laboratory Science
- Clinical Support
- Culinary and Hospitality
- Culture
- EVS
- Featured Articles
- General Management
- Human Resources
- Imaging
- Inclusion and Belonging
- Information Technology
- Mentorship
- Nursing
- Operations
- Patient and Customer Experience
- Pharmacy
- Rehabilitation Services
- Revenue Cycle
- Social Services
- Students and Internships
- Veterans
- Wellness & Benefits
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019

Kimouy Williams on Delivering Passionate Care as a PCA
As a patient care associate (PCA) at Long Island Jewish Medical Center, Kimouy Williams spends each day with our patients putting all she has into helping make their time at Northwell Health a little more comfortable.
Even when her day consists of wearing multiple hats, Kimouy is eager to greet and attend to each patient, assisting them in getting up, bathed, dressed, and ensuring that they have all they need to be comfortable throughout the day. “I always make sure my clients have snacks and a clean bedside table. I know the effects that hunger can have on a patient’s mood and being attentive with cleanliness is an important part of being a successful PCA.”
A patient care associate is a fulfilling career that Kimouy truly cherishes. “My career at Northwell is something that I’m very proud of. I’m excited to continue my journey here and being given the opportunity to advance my education in nursing while working with incredibly dedicated healthcare professionals who are committed to providing the best care to every person who walks through our doors”, shared Kimouy when asked why she loves working at Northwell.
When Kimouy left Jamaica and came to the US almost five years ago, she knew she wanted to pursue her passion in caring for others like she did for her late grandmother, who taught her so much about hard work and perseverance. “These traits are very much a requirement for me to succeed in my role. Choosing a career at Northwell was an easy decision because they not only offer amazing benefits, they also support my dreams of furthering my career in healthcare.”
Join Kimouy and the incredible nursing support team in a career well cared for at Northwell. Apply today!
Newsletter
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Recent Posts
- Explore two different career paths beginning as a nurse extern at Northwell Health.
- Mentorship, desired career growth, and making a difference: Meet Christopher, emergency department registered nurse
- Explore career paths in pharmacy at Northwell Health.
- From quality to operations: Discover Shivani’s career journey in labs
- Discover Tyler’s career journey in facilities and support services at Northwell Health
Categories
- Academia and Research
- Administrative Support
- Advance Clinical Providers
- Business
- Career Advice
- Career Paths
- Clinical Care
- Clinical Laboratory Science
- Clinical Support
- Culinary and Hospitality
- Culture
- EVS
- Featured Articles
- General Management
- Human Resources
- Imaging
- Inclusion and Belonging
- Information Technology
- Mentorship
- Nursing
- Operations
- Patient and Customer Experience
- Pharmacy
- Rehabilitation Services
- Revenue Cycle
- Social Services
- Students and Internships
- Veterans
- Wellness & Benefits
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019

Northwell Celebrates: A series of events and experiences celebrating and thanking our healthcare heroes and their families
It’s not often that we’re faced with taking on challenges on a global scale such as was the case with the pandemic. In moments such as those, it’s important to pull together to raise each other. That is exactly what employees at Northwell Health did. They raised health, raised communities, and through it all they raised each other.
A simple thank you wasn’t enough. Northwell wanted to celebrate and thank all employees for their courage, determination and dedication throughout the pandemic and every day. Northwell Celebrates was launched as a multi-faceted token of appreciation. It is a series of events, activities and experiences curated for the enjoyment of employees and their families throughout the year.
Included in these activities are pop-up gratitude stations at various Northwell facilities where executive leaders from across the health system participate to give their personal thanks and offer a well-being gift box to employees. David Gill, assistant vice president of Employee Experience, was among the leadership present at the Syosset Hospital gratitude pop-up. David says, “It’s a way for us to provide in-person recognition and appreciation for the work our team members continue to do every day to make Northwell a great place to work and receive care.”
Inside each gift box are essentials to self-care such as a candle, a weekly reflection journal, a mindfulness coloring book with colored pencils, among other items. Such a gift was not taken lightly by employees like Elise Yan, lead lab technologist at Long Island Jewish Forest Hills, who took to Facebook: “Thank you Northwell LIJ Forest Hills! Love it, can’t wait to start using them!”
Other events are planned throughout the summer, like drive-in family movie nights, a family fun book, concerts and an invitation to have six free chef-prepared meals from Freshly delivered directly to employees’ homes. The Freshly deliveries were a huge hit, with employees like Audrey McCullough, assistant director of patient care services for the Division of Nursing, who hopped on social media to say, “Thanks, Northwell, you really have my heart. Just received my 6 free and healthy, chef-cooked meals delivered right to my doorstep by Freshly!!”
At Northwell, all employees are valued and their hard work never goes unnoticed.
Discover a career well cared for at Northwell Health.
Share this entry
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Recent Posts
- Explore two different career paths beginning as a nurse extern at Northwell Health.
- Mentorship, desired career growth, and making a difference: Meet Christopher, emergency department registered nurse
- Explore career paths in pharmacy at Northwell Health.
- From quality to operations: Discover Shivani’s career journey in labs
- Discover Tyler’s career journey in facilities and support services at Northwell Health
Categories
- Academia and Research
- Administrative Support
- Advance Clinical Providers
- Business
- Career Advice
- Career Paths
- Clinical Care
- Clinical Laboratory Science
- Clinical Support
- Culinary and Hospitality
- Culture
- EVS
- Featured Articles
- General Management
- Human Resources
- Imaging
- Inclusion and Belonging
- Information Technology
- Mentorship
- Nursing
- Operations
- Patient and Customer Experience
- Pharmacy
- Rehabilitation Services
- Revenue Cycle
- Social Services
- Students and Internships
- Veterans
- Wellness & Benefits
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019

Discovering unlimited opportunities and a true calling — meet Elyse Isopo
Elyse Isopo started her Northwell Health career journey as a junior volunteer at North Shore University Hospital (NSUH) when she was in high school. “I loved the people, I loved the patients, and I love helping,” she says. Today, she is a supervisor for advanced clinical providers (ACP) at NSUH, where she oversees a team of nurse practitioners and physician assistants.
As a volunteer in high school, Elyse became immersed in a hospital environment and patient care as she delivered their newspapers, refilled their water, and transported them, while also helping with art and music programs. The experience impacted her career path. “I always knew I wanted to be a nurse,” she says.
Elyse held many roles during her 22 years at NSUH. She started as a registered nurse on a medicine unit and then transitioned to the medical intensive care unit (MICU). “After becoming a nurse, I knew I wanted to extend my career within the nursing field.” With the assistance of Northwell’s tuition reimbursement, Elyse went back to school to become a family nurse practitioner. “Northwell encourages and financially assists education and advancement of one’s career,” she says. Once Elyse obtained her master’s degree as a nurse practitioner, she transitioned into presurgical testing (PST). After five years on the PST unit, Elyse realized her heart was always with critical care, so she returned to the MICU where she’s worked for the past 14 years.
A driven nurse practitioner committed to learning and growth, Elyse earned her second master’s as an acute care nurse practitioner — and with Northwell’s support, she received tuition reimbursement for her doctorate of nursing practice (DNP) as well. To share her passion for nursing with others, she became a professor at Hofstra University as an adjunct clinical faculty member, where she supervises clinical faculty in the nurse practitioner programs. As a nurse and nurse practitioner, Elyse is involved with patient and family education. “I found a love of teaching throughout my career when I am precepting new nurses; teaching ACPs, residents and interns; and speaking with patients and their families.”
Reflecting on her tenure at NSUH, Elyse says, “You don’t have just a hospital, you have a community.” During COVID and as a frontline health worker, Elyse never considered herself a hero, but once she stepped outside the hospital for a “clap-out” from local first responders — whose ladder trucks erected an arch under which NSUH staff walked as they were applauded — she was reminded that her career was more than a job; it was a true calling. “I didn’t want to be anywhere else.”
At Northwell, we strive to have our team members continue their career and education journey. Elyse is proof of that: “Northwell helps build each of us to our greatest potential professionally no matter what your career trajectory is.”
Discover a career well cared for and explore nursing opportunities.
Share this entry
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Recent Posts
- Explore two different career paths beginning as a nurse extern at Northwell Health.
- Mentorship, desired career growth, and making a difference: Meet Christopher, emergency department registered nurse
- Explore career paths in pharmacy at Northwell Health.
- From quality to operations: Discover Shivani’s career journey in labs
- Discover Tyler’s career journey in facilities and support services at Northwell Health
Categories
- Academia and Research
- Administrative Support
- Advance Clinical Providers
- Business
- Career Advice
- Career Paths
- Clinical Care
- Clinical Laboratory Science
- Clinical Support
- Culinary and Hospitality
- Culture
- EVS
- Featured Articles
- General Management
- Human Resources
- Imaging
- Inclusion and Belonging
- Information Technology
- Mentorship
- Nursing
- Operations
- Patient and Customer Experience
- Pharmacy
- Rehabilitation Services
- Revenue Cycle
- Social Services
- Students and Internships
- Veterans
- Wellness & Benefits
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019

How discipline and a call to service propelled veteran Cynthia LaRocca’s successful career at Northwell Health
Serving country and community always came naturally to Cynthia LaRocca, director of clinical professional development at Plainview and Syosset Hospitals.
As a member of the U.S. Army Reserve, Cynthia served in a variety of roles including pharmacy technician and field medic. Her military path led to jobs at VA hospitals in Brooklyn, Philadelphia and Nebraska—experiences where “I found nursing and nursing found me.”
Cynthia’s transition to a civilian career at Northwell was eased by lessons learned during her eight years in the reserve. “Discipline is a skill that I have learned from the military and that serves me well at Northwell because it means seeing something through from beginning to end.”
In addition, the teamwork skills she acquired in the military translated easily to the Northwell Health value of being Truly Together: whether serving the country or serving the community, she says, “without your colleagues you cannot achieve your ultimate goals or complete your mission.”
Today, Cynthia manages the clinical professional development of orientations, annual training skills, new equipment and professional acumen for the clinical nursing staff at both Plainview and Syosset Hospitals. And by embodying the Northwell Health value of Truly Ambitious, she has seized opportunities to spread her wings and redefine what it means to work in health care, reaching career goals and achieving credentials including registered nurse (RN), registered nurse–board certified (RNBC) and doctor of nursing practice (DNP).
Work excites Cynthia every day because “I know what I am doing is helping others,” and appreciates that Northwell prioritizes ensuring all military employees feel supported, whether they continue to serve while on the job or are veterans who have completed their service: “The support Northwell gives to those who serve cannot be understated.”
Apply the lessons you learned in the military toward a Northwell Health career. Discover a career well cared for.
Share this entry
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Recent Posts
- Explore two different career paths beginning as a nurse extern at Northwell Health.
- Mentorship, desired career growth, and making a difference: Meet Christopher, emergency department registered nurse
- Explore career paths in pharmacy at Northwell Health.
- From quality to operations: Discover Shivani’s career journey in labs
- Discover Tyler’s career journey in facilities and support services at Northwell Health
Categories
- Academia and Research
- Administrative Support
- Advance Clinical Providers
- Business
- Career Advice
- Career Paths
- Clinical Care
- Clinical Laboratory Science
- Clinical Support
- Culinary and Hospitality
- Culture
- EVS
- Featured Articles
- General Management
- Human Resources
- Imaging
- Inclusion and Belonging
- Information Technology
- Mentorship
- Nursing
- Operations
- Patient and Customer Experience
- Pharmacy
- Rehabilitation Services
- Revenue Cycle
- Social Services
- Students and Internships
- Veterans
- Wellness & Benefits
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
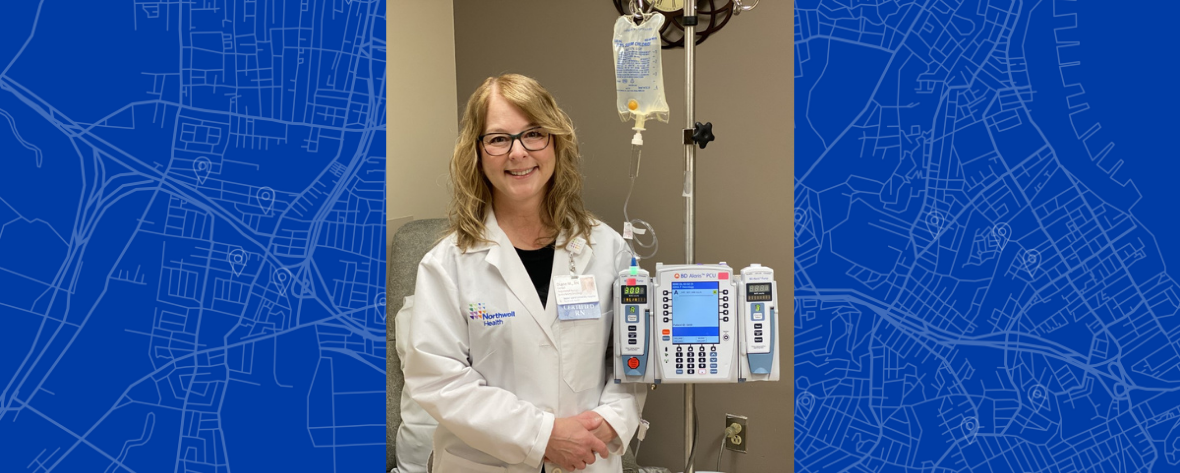
Continuing her growth and creating unforgettable memories—meet Diane Geraci RN, BSN, OCN
In honor of Nurses Week, which Northwell Health is celebrating throughout May, we are highlighting some of our amazing nurses as they share stories about their careers, growth and experiences. Throughout her 36 years as a registered nurse at Staten Island University Hospital (SIUH), Diane Geraci has achieved both professional and personal growth.
Continuing her education and evolving her skillset
Diane started her nursing career journey in 1985 as a graduate nurse at SIUH. “It was my favorite hospital to do the clinical rotations,” she says. From her first days at SIUH, she knew she would grow and learn within the same hospital.
“Northwell and SIUH have been very supportive of my growth,” Diane says of a career that’s included roles in rehab/orthopedic surgery, the operating room and ambulatory oncology.
Because continuing education is very important to Diane, leadership encouraged her to enroll in oncology certification courses and offered tuition reimbursement for a Bachelor of Science in Nursing at the College of Staten Island. “It took four years and a lot of hard work, and I graduated with a BSN—and all thanks to the ease of the program because of Staten Island University Hospital. I’m so thankful for their encouragement and financial support!”
Not only did Diane receive her BSN, she also obtained her nursing certification in oncology and immunotherapy to further her knowledge in her field.
From Harvey to hockey: experiences she’ll never forget
In August 2017, Hurricane Harvey made a Category 4 landfall in Texas, devastating much in its path. Northwell quickly assembled a medical mission team to assist at MD Anderson Cancer Center in Houston. When Diane received the email about the catastrophe, she immediately volunteered to go!
“MD Anderson Cancer Center needed oncology nurses who were certified and who had a chemotherapy/immunotherapy certification, and thanks to SIUH I was certified in both,” she says. “The MD Anderson staff was great to work with, and I met so many cancer patients from all around the world. This truly was one of the highlights of my career.”
When Diane and her team returned home—with indelible memories from the front lines of care—they were greeted with a dinner reception and the opportunity to meet Michael Dowling. “I thank these two hospitals for their generosity to the teams, and for Northwell helping out a devastated community in another state.”
Another unforgettable moment of Diane’s career at SIUH was winning Northwell’s ”Win it Wednesdays” contest, a weekly prize drawing hosted by Northwell’s internal communications team on the Northwell Life Facebook page. What made it unforgettable wasn’t just the fact she won—it was what happened next.
Diane’s prize was a lavender, official New York Rangers hockey jersey. The jersey was too big, so she wanted to give it to a hockey fan. Her floor and nurse manager alerted her that there was a teenage boy—a big Rangers fan—who wanted a jersey as part of his Make-A-Wish request. “He was being treated for lymphoma on the pediatric oncology unit, which was right next to my unit,” says Diane, who met the boy and gave him the jersey!
When the social workers within the unit heard about Diane’s gracious act, they reached out to the team and received box seat tickets for the patient’s family to attend a home game! “It was meant to be,” she says.
Reflecting on her fulfilling career, Diane says, “Northwell is a great place to work! I feel well supported and encouraged to continue my growth with nursing and create more memories.”
Share this entry
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Recent Posts
- Explore two different career paths beginning as a nurse extern at Northwell Health.
- Mentorship, desired career growth, and making a difference: Meet Christopher, emergency department registered nurse
- Explore career paths in pharmacy at Northwell Health.
- From quality to operations: Discover Shivani’s career journey in labs
- Discover Tyler’s career journey in facilities and support services at Northwell Health
Categories
- Academia and Research
- Administrative Support
- Advance Clinical Providers
- Business
- Career Advice
- Career Paths
- Clinical Care
- Clinical Laboratory Science
- Clinical Support
- Culinary and Hospitality
- Culture
- EVS
- Featured Articles
- General Management
- Human Resources
- Imaging
- Inclusion and Belonging
- Information Technology
- Mentorship
- Nursing
- Operations
- Patient and Customer Experience
- Pharmacy
- Rehabilitation Services
- Revenue Cycle
- Social Services
- Students and Internships
- Veterans
- Wellness & Benefits
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019

What Nicole Natale Learned on the Frontlines During the Pandemic
In honor of Nurses Week, which Northwell Health is celebrating throughout May, we are highlighting some of our amazing nurses as they share stories about their careers, challenges, and experiences. Nicole Natale faced one of her greatest challenges early in her career and her experience on the frontlines during the COVID-19 pandemic has shaped friendships, as well as her understanding of what it means to be a nurse.
Currently a registered nurse at North Shore University Hospital (NSUH) in the Neurosurgical Intensive Care Unit (ICU), Nicole Natale began her career in 2017, as a nurse extern at Huntington Hospital. Nicole fell in love with critical care after experiencing the various facets of nursing care while floating from the emergency room and ICU, to the medical-surgical and pediatrics floors during nursing school.
As fate would have it, Nicole was invited to interview with the Neurosurgical ICU at NSUH shortly after losing her aunt to glioblastoma brain cancer just before graduation. The loss of her aunt to brain cancer left Nicole feeling like she was destined to work with neurosurgical patients.
After successfully landing her dream job at NSUH, Nicole’s budding career took an unexpected turn. After she finished the critical care fellowship orientation, the world was suddenly turned upside down as the COVID-19 pandemic began. Being a new graduate in a global pandemic was one of the most challenging obstacles Nicole has ever faced, but she credits the support of her coworkers, her managers, and Northwell leadership for making the experience less tumultuous. As Nicole put it, “Northwell made me feel safe, cared for, and supported, and I am forever grateful to work for this health system.”
Despite the incredible hardships, the experience was invaluable, as Nicole learned so much so quickly. Her coworkers became her role models and her support system as they leaned on one another to survive. “It was such a scary time for all of us. Working in a COVID unit feels like you’re in a battlefield. Working in these conditions brought my work team together and the bonds I have with my coworkers grew so strong that they are like family to me.”
It is this level of support that Nicole cites as one of the many reasons she would encourage anyone to work at Northwell given the opportunity. Examples of the support she receives from Northwell include career growth with clinical ladder and research committees and physical and mental well-being with things like the Lavender Room where staff can relax and unwind. Northwell is proud to advocate for its nurses and all of our team members, at every step of their journey.
Explore nursing opportunities and learn more about a career well cared for at a Fortune 100 Best Companies to Work For®
Share this entry
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Recent Posts
- Explore two different career paths beginning as a nurse extern at Northwell Health.
- Mentorship, desired career growth, and making a difference: Meet Christopher, emergency department registered nurse
- Explore career paths in pharmacy at Northwell Health.
- From quality to operations: Discover Shivani’s career journey in labs
- Discover Tyler’s career journey in facilities and support services at Northwell Health
Categories
- Academia and Research
- Administrative Support
- Advance Clinical Providers
- Business
- Career Advice
- Career Paths
- Clinical Care
- Clinical Laboratory Science
- Clinical Support
- Culinary and Hospitality
- Culture
- EVS
- Featured Articles
- General Management
- Human Resources
- Imaging
- Inclusion and Belonging
- Information Technology
- Mentorship
- Nursing
- Operations
- Patient and Customer Experience
- Pharmacy
- Rehabilitation Services
- Revenue Cycle
- Social Services
- Students and Internships
- Veterans
- Wellness & Benefits
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019

Driven and Determined Nicole Martinez, RN
In honor of Nurses Week, which Northwell Health is celebrating all month long, we are sharing the stories of some of our incredible nurses and their inspirational journeys. For Nicole Martinez, she decided to become a nurse all because of a smile.
It all began when her mother was being cared for at Long Island Jewish Medical Center (LIJMC) for pancreatic cancer in 2005. Although her mother’s outcome was not the one Nicole’s family had hoped for, the amazing nurses, doctors and patient care assistants left a lasting impression. The day Nicole was told her mother only had one week to live, she walked into the room expecting tears but instead found her mother smiling with her nurse. Reflecting on that moment, Nicole says, “To this day I do not know what that nurse said to make her smile, but I remember thinking here is a 46-year-old woman who was just told she was going to die…and someone made her smile.” That moment and that smile was what led Nicole to become a nurse so that she too could help others find comfort during the most difficult time in their lives.
After her mother passed away, Nicole needed to pause her education to help support her family, so she took a position as a receptionist at LIJMC where she worked for two years before applying and being accepted to nursing school. With the support of Northwell, her manager, and her coworkers, Nicole was able to continue working full time while attending school full time with support from Northwell’s tuition reimbursement program. Her determination and hard work paid off when she graduated with her Associate Degree in Nursing and began working as a registered nurse on the same floor where she was a receptionist. But she wasn’t finished yet. Nicole went on to complete her Bachelor of Science in Nursing, once again aided by tuition reimbursement and encouragement from Northwell. But she still wasn’t finished. After transferring to the Ambulatory Surgery Unit, (ASU), Nicole again set her sights a little higher and completed her master’s degree. She was then promoted to her current role of assistant nurse manager.
About her amazing accomplishments, Nicole says, “Northwell gave me the opportunities, the strength, the financial support, and the courage that I needed to attain my goals. I tell everyone to this day if you want it, there is no excuse. Thank you Northwell for the past 15 years. Because of you, I am who I am today!”
Share this entry
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Recent Posts
- Explore two different career paths beginning as a nurse extern at Northwell Health.
- Mentorship, desired career growth, and making a difference: Meet Christopher, emergency department registered nurse
- Explore career paths in pharmacy at Northwell Health.
- From quality to operations: Discover Shivani’s career journey in labs
- Discover Tyler’s career journey in facilities and support services at Northwell Health
Categories
- Academia and Research
- Administrative Support
- Advance Clinical Providers
- Business
- Career Advice
- Career Paths
- Clinical Care
- Clinical Laboratory Science
- Clinical Support
- Culinary and Hospitality
- Culture
- EVS
- Featured Articles
- General Management
- Human Resources
- Imaging
- Inclusion and Belonging
- Information Technology
- Mentorship
- Nursing
- Operations
- Patient and Customer Experience
- Pharmacy
- Rehabilitation Services
- Revenue Cycle
- Social Services
- Students and Internships
- Veterans
- Wellness & Benefits
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019

How We Celebrated Our Nursing Health Raisers During Nurses Week!
National Nurses Week is here and at Northwell Health we are celebrating every moment of it. In fact, we will be celebrating all month long to honor our 18,000+ nurses across Long Island, Manhattan, Queens, Staten Island and Westchester. After a year unlike any other, we are stronger today because of our registered nurses’ commitment to raising the standard of care in the communities where we live, love and belong. And as we reflect on the selfless individuals the whole world considers heroes, it fills our hearts with gratitude to call these incredible men and women our colleagues, our friends, our family, and our neighbors.
During Nurses Week, Northwell has many activities planned to honor our nurses including, virtual cooking classes, blessing of the hands, award ceremonies, wellness initiatives such as yoga and wellness retreats, among other activities.
Hear why our nurses in their own words love working at Northwell and how they feel supported.
“Endless opportunities to shoot for the stars.”
“I love working as a nurse with Northwell because its more than a job, it’s a family. The support, the encouragement, the camaraderie, and the overall feeling that you are part of a team making a difference in people’s lives.”
“There are so many opportunities for a nurse at Northwell. Follow your passion and seek new challenges.”
“The fact that I’ve been a nurse at LIJ Medical Center since 1980, way before it was Northwell, speaks of my trust and dedication!”
“I love being a nurse at Northwell because I have the pleasure of working and meeting people with diverse backgrounds to improve the health of our communities.”
“Being a Northwell nurse is like having a second family and a home. Great teamwork, support, a safe place to work and my voice is heard. I like Northwell’s values and commitment to our patients and community.”
“I love being a Northwell nurse because I work with a great interdisciplinary team. Northwell supports my career advancement and continuing education.”
“Compassion amongst team members to provide the best care possible for our patients.”
“I love the ability to work in all different areas of nursing and be able to stay with a system who supports me.”
“I work with a phenomenal group of nurses who never hesitate to help one another, and who I consider to be my friends. We’ve all been working away on the COVID floor, staying strong for our patients and each other.”
“Because you come to realize at some point in your career that nurses are a powerful group that can affect and guide change. Our patients and our communities deserve the voice we can give them.”
Join our team members and discover a career well cared for. Apply today!
Share this entry
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Recent Posts
- Explore two different career paths beginning as a nurse extern at Northwell Health.
- Mentorship, desired career growth, and making a difference: Meet Christopher, emergency department registered nurse
- Explore career paths in pharmacy at Northwell Health.
- From quality to operations: Discover Shivani’s career journey in labs
- Discover Tyler’s career journey in facilities and support services at Northwell Health
Categories
- Academia and Research
- Administrative Support
- Advance Clinical Providers
- Business
- Career Advice
- Career Paths
- Clinical Care
- Clinical Laboratory Science
- Clinical Support
- Culinary and Hospitality
- Culture
- EVS
- Featured Articles
- General Management
- Human Resources
- Imaging
- Inclusion and Belonging
- Information Technology
- Mentorship
- Nursing
- Operations
- Patient and Customer Experience
- Pharmacy
- Rehabilitation Services
- Revenue Cycle
- Social Services
- Students and Internships
- Veterans
- Wellness & Benefits
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019

Recognizing our skilled nursing facility team members
As National Skilled Nursing Care Week is approaching, Northwell Health would like to recognize the dedicated and compassionate care of our skilled nursing care facilities. Our skilled nurses and certified nurse assistants provide the highest quality care to patients requiring both long-term and short-term care.
Meet some of our team members from the Orzac Center for Rehabilitation:
Alice Caressimo, Registered Nurse
As a registered nurse, Alice’s role is to educate her patients and their families about her patient’s health and help discuss their plan of care. “My work experience with Orzac has been very rewarding,” says Alice. “The compassion and support from the nursing managers and nursing staff I feel is what makes us a great team and contributes to the excellent care we strive to provide.”
Courtney Caldero, Registered Nurse
Working as a registered nurse at Orzac, Courtney not only takes care of rehab patients but she is also a long-term care and hospice nurse. Her daily responsibilities involve wound care, pain management, patient and family advocacy, safe medication administration, and patient safety. She is a proud nurse who loves her job and finds it very rewarding. “You are more than just a nurse,” says Courtney. “You are your patient’s and their family’s sense of comfort–their educator and ears. The profession is not easy by any means but being able to assist and support people through what is the most difficult time of their life is what’s beyond rewarding.”
Nina Bianco, Registered Nurse
As a registered nurse, Nina believes her patient’s physical, mental, and spiritual wellbeing is priority. She performs an age-specific plan of care based on the individual needs of each patient. Within her first year working as a new nurse during a global pandemic, Nina was supported by her team through every step. “Working together as a team and effective communication are the essentials for providing quality health care and safety.”
Donna Douglas, Certified Nurse Assistant
As a certified nurse assistant, Donna’s role is to provide the patient with the most dignifying care, and assist with their Activities of Daily Living to help them feel strong and confident enough to return to their community. “Working in my facility is extremely rewarding because I gain new perspective on aging. I also get an opportunity to interact with patients daily during a difficult time in their lives when they are away from their family and in a new environment,” says Donna. “I try my best every day to make this tough experience as easy and rewarding for the patient as I can.”
 Andrea McDonald, Certified Nurse Assistant
Andrea McDonald, Certified Nurse Assistant
Working as a certified nurse assistant, Andrea provides compassionate care to her patients. Her responsibilities include direct patient care and putting a smile on their face! Her favorite thing about her job is her team who go the extra mile for their patients. “I find working at my facility rewarding because my team is pleasant and competent and I have professional, caring managers,” says Donna.
Share this entry
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Recent Posts
- Explore two different career paths beginning as a nurse extern at Northwell Health.
- Mentorship, desired career growth, and making a difference: Meet Christopher, emergency department registered nurse
- Explore career paths in pharmacy at Northwell Health.
- From quality to operations: Discover Shivani’s career journey in labs
- Discover Tyler’s career journey in facilities and support services at Northwell Health
Categories
- Academia and Research
- Administrative Support
- Advance Clinical Providers
- Business
- Career Advice
- Career Paths
- Clinical Care
- Clinical Laboratory Science
- Clinical Support
- Culinary and Hospitality
- Culture
- EVS
- Featured Articles
- General Management
- Human Resources
- Imaging
- Inclusion and Belonging
- Information Technology
- Mentorship
- Nursing
- Operations
- Patient and Customer Experience
- Pharmacy
- Rehabilitation Services
- Revenue Cycle
- Social Services
- Students and Internships
- Veterans
- Wellness & Benefits
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019

Get to know our team members behind the scenes during Medical Laboratory Professionals Week
This week Northwell Health is celebrating Medical Laboratory Professionals Week! Our Medical Laboratory professionals play a vital role within our organization by providing crucial information for detecting, diagnosing, treating, and monitoring a patient’s disease. They are our healthcare heroes behind the scenes!
Meet some of our team members:
Ryan Brenkret, Lead Cytology Technologist, Anatomic Pathology Services, Division of Cytology
Working as a lead cytology technologist, Ryan’s primary role is to screen and diagnose cytology cases using a light microscope to look mainly for cancer, infectious diseases, as well as other inflammatory conditions which people may suffer from. “My favorite thing about my career is trying to figure out what the patient has and provide a quality diagnosis, says Ryan. “We as cytologists really have the power to help the patients by providing accurate diagnoses or also by detecting a patient’s cancer in the early stage. Then they can receive the proper, life-saving treatments.”
 Daisey Williams, Pathology Histology Technician, Staten Island University Hospital North
Daisey Williams, Pathology Histology Technician, Staten Island University Hospital North
As a histology technician Daisey plays a crucial role in the diagnosis and treatment of diseases, by turning tissue samples into microscopic slides. Leadership has been a constant role model and support system for Daisey where she can voice her opinions and ideas. “My favorite part of this field is knowing that my work can provide our patients with a diagnosis and aide in their treatment and their next steps to recovery,” says Daisey.
 Sean Houston, Clinical Lab Technologist, Automated Lab
Sean Houston, Clinical Lab Technologist, Automated Lab
As a lab technologist, Sean is responsible for running general immunoassay chemistry and drugs of abuse testing on the state-of-the-art, automated Roche line. Sean is within his first year at Northwell and he is looking forward to continuous growth within the organization and laboratory field. His favorite thing about working as a lab technologist? “I enjoy working alongside my diverse and well-skilled team!”
 Christina Mikell, Medical Laboratory Technologist, Histology, Plainview Hospital
Christina Mikell, Medical Laboratory Technologist, Histology, Plainview Hospital
In Christina’s role, she aides in the processing of surgical tissue specimens. This is where they would chemically preserve the tissue so that they can then embed, cut, and stain representative sections on microscope slides. Within her role, she also performs specialty stains on slides that can help identify certain diseases and/or infections. As a new graduate, Christina has learned many skills within the pathology lab that will help her grow in her career. “My favorite thing about working as a lab tech in the histology department is the hands-on creative work that we get to perform every day,” says Christina. “I am able to take my technical knowledge and create something that can really be seen as beautiful.”
 Michael Desimone, Histology Pathology Assistant, North Shore University Hospital
Michael Desimone, Histology Pathology Assistant, North Shore University Hospital
Working as a pathologist assistant, Michael partakes in high-quality patient care primarily through macroscopic evaluation, examination, and dissection of all surgical pathological specimens that come through the lab. Apart of being a pathologist assistant, Michael has enjoyed growing as an educator for pathology residents, pathologist assistant students, and medical technologist students. “We’re able to bring a pathologic process that a student once learned in a classroom and connect it with a real-life patient and specimen, with real implications for care,” says Michael. “I take a particular pride in teaching students and residents important details in macroscopic examination that make a large difference for cancer staging.”
 Alexa Duque, Anatomical, Pathology Assistant, Lenox Hill Hospital
Alexa Duque, Anatomical, Pathology Assistant, Lenox Hill Hospital
As a pathologist assistant, Alexa facilitates the diagnostic process by providing a comprehensive macroscopic examination and evaluation of all surgical pathological specimens. Alexa started her Northwell career journey two years ago and has grown into her role by supporting the lab in different areas. One example includes assisting her supervisor with process improvements which allowed her to gain new skills and insight. “I love that it is primarily hands on and that I get to appreciate the fascinating anatomy of the human body while being able to help patients behind the scenes,” says Alexa.
 Roby P. Raju, Supervisor, Clinical Laboratory Operations, Center for Advanced Medicine
Roby P. Raju, Supervisor, Clinical Laboratory Operations, Center for Advanced Medicine
As a supervisor in his role, Roby oversees the day-to-day laboratory operations for his team. He ensures the laboratory maintains and follows compliance standards and regulations set by both accrediting and government agencies. “My favorite thing about being a laboratory technologist is that I am proud of the results we provide to the physicians and nurses from our laboratory,” says Roby.
Became a Health Raiser and discover a career well cared for, explore clinical laboratory careers. Apply today!
Share this entry
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Recent Posts
- Explore two different career paths beginning as a nurse extern at Northwell Health.
- Mentorship, desired career growth, and making a difference: Meet Christopher, emergency department registered nurse
- Explore career paths in pharmacy at Northwell Health.
- From quality to operations: Discover Shivani’s career journey in labs
- Discover Tyler’s career journey in facilities and support services at Northwell Health
Categories
- Academia and Research
- Administrative Support
- Advance Clinical Providers
- Business
- Career Advice
- Career Paths
- Clinical Care
- Clinical Laboratory Science
- Clinical Support
- Culinary and Hospitality
- Culture
- EVS
- Featured Articles
- General Management
- Human Resources
- Imaging
- Inclusion and Belonging
- Information Technology
- Mentorship
- Nursing
- Operations
- Patient and Customer Experience
- Pharmacy
- Rehabilitation Services
- Revenue Cycle
- Social Services
- Students and Internships
- Veterans
- Wellness & Benefits
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
Click here to add your own text

From EMT to nurse, career growth at Northwell can take you in many directions
Career growth means different things to different people. At Northwell Health, we support all our team members’ career growths and aspirations, whether they are growing in their current role, taking their career on a different path, or expanding their skills with continued education. Meet Colleen McKenna who experienced her own career growth at Northwell that began as an Emergency Medical Technician (EMT) and continued in nursing.
Her Northwell career began in 2015 as an EMT, where Colleen developed skills to stabilize and transport patients who are in need of emergency medical care. Within a year, she completed a paramedic program at Northwell Health’s Center for Learning and Innovation and was promoted into a new role as a paramedic.
As both an EMT and paramedic, Colleen was exposed to direct patient care that inspired her to pursue a nursing career. From that time, she knew that she wanted to provide those skills to her community. “I have always been the type of person that wants to help others and make a difference,” says Colleen.
As Colleen’s determination and passion for patient care grew, she received much support from her leaders to pursue her interest in nursing. She enrolled in prerequisites for a nursing program and was able to continue to work as a paramedic while going to school. With the support of Northwell’s tuition reimbursement program, Colleen obtained her Associate of Applied Science in Nursing. As her education journey continues, Colleen was accepted into the Farmingdale State College nursing program. “The support from leadership has been amazing. My direct supervisor checks in with me frequently to ensure I am on the right path to achieve my career goals.”
This upcoming December, Colleen will be completing her Bachelor of Science in Nursing degree and is looking forward to becoming a registered nurse at Northwell. “Northwell Health is a great company to work for because the opportunity for growth is endless and the health system provides you with all of the necessary tools to help you achieve your goals.”
Discover a career well cared for at Northwell Health. Apply today!
Share this entry
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Recent Posts
- Explore two different career paths beginning as a nurse extern at Northwell Health.
- Mentorship, desired career growth, and making a difference: Meet Christopher, emergency department registered nurse
- Explore career paths in pharmacy at Northwell Health.
- From quality to operations: Discover Shivani’s career journey in labs
- Discover Tyler’s career journey in facilities and support services at Northwell Health
Categories
- Academia and Research
- Administrative Support
- Advance Clinical Providers
- Business
- Career Advice
- Career Paths
- Clinical Care
- Clinical Laboratory Science
- Clinical Support
- Culinary and Hospitality
- Culture
- EVS
- Featured Articles
- General Management
- Human Resources
- Imaging
- Inclusion and Belonging
- Information Technology
- Mentorship
- Nursing
- Operations
- Patient and Customer Experience
- Pharmacy
- Rehabilitation Services
- Revenue Cycle
- Social Services
- Students and Internships
- Veterans
- Wellness & Benefits
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019

Healthcare workers reflect on one year of delivering care throughout the COVID-19 pandemic
March marked one year of our Northwell Health team members delivering care throughout the COVID-19 pandemic, a disease that has impacted our world on an unprecedented level. While the past year has been like no other, our team members have come together to become health raisers. Throughout it all, they have been a bright light of hope amidst some of the darkest times. We asked our team members to take a moment to reflect on their thoughts and feelings on what the past year has meant for them and how they’ve grown.
Read the reflections of our healthcare heroes:
“I am forever changed as a healthcare professional. It was difficult watching all of our patients come into the hospital alone without the support of their families. It has changed me as a nurse to also be their support system and make being in the hospital less scary for them.”
“I have learned that I need to take time for self-care in order to be a better me, including a better ‘work me’. I’m really happy our workplace supports that.”
“I learned that we are able to fight anything. Northwell has made us all strong in fighting this pandemic. We learned to take care of ourselves along with our patients and we will continue to Raise Health.”
“Throughout the past year, we’ve been inspired by our patients. Their recovery is our recovery. Their hope is our hope. In those dark times they were beams of light. Together we will persevere.”
“I have learned to really appreciate the impact we make for our patients, even working remote or in an office. COVID reminded us of the role each and every one of us has in helping patients get better.”
“This past year has shown me how awesome my Northwell coworkers are. When faced with challenges, we rise to the occasion. I am still in awe of the dedication and compassion they have not only shown the patients but each other as well. I hope to never face a healthcare challenge like this again, but I take comfort in knowing that my Northwell family will be there to get us through it!”
“My whole life has changed tremendously since last March. Since being redeployed from my role as a standardized patient, I have worked with Workforce Safety on mask fit testing, met the nurses and support staff at different hospitals, mobile units and vaccine pods, and came to know church leaders in faith-based testing. With the unflagging, determined and courageous support of our outstanding Community Relations team, I and many others like me have had our eyes opened to the tremendous amount of goodwill, generosity of spirit, and all-encompassing empathy that our Northwell family possesses – and we are all so much the better for it.”
“Scientists and researchers are ‘behind the scenes’ healthcare heroes and this year I felt even more proud of being a medical researcher. It was empowering to see how the complex biology questions scientists spent time understanding and the knowledge/techniques they discovered eventually came together to produce and distribute the vaccines that are giving us hope that we can end this.”
“Being a respiratory therapist over this past year, in the height of a pandemic, has taught us to be creative in problem solving, to provide the bestcare for our patients during uncertain times and promote a positive working environment during the darkest hours. It has taught me the ability to positively influence coworkers and teammates to work together for a common cause and mission.”
“As an MRI radiology manager, my job changed dramatically (during COVID) as we focused on keeping patients safe during MRIs. COVID has given me a greater sense of pride than anything else I dealt with in over 20 years of my career. As a leader I watched my team step up in ways that I couldn’t imagine.”
“These unprecedented times have changed me as a healthcare hero in that I have gained a tremendous amount of respect for every single role within the system. I have witnessed heroism from everyone and I feel lucky to play a small role in a community that exudes cohesiveness, unity and respect – which was so palpable throughout the past year.”
Join our team members as they Raise Health in the communities where we live, love and work. Apply today!
Share this entry
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Recent Posts
- Explore two different career paths beginning as a nurse extern at Northwell Health.
- Mentorship, desired career growth, and making a difference: Meet Christopher, emergency department registered nurse
- Explore career paths in pharmacy at Northwell Health.
- From quality to operations: Discover Shivani’s career journey in labs
- Discover Tyler’s career journey in facilities and support services at Northwell Health
Categories
- Academia and Research
- Administrative Support
- Advance Clinical Providers
- Business
- Career Advice
- Career Paths
- Clinical Care
- Clinical Laboratory Science
- Clinical Support
- Culinary and Hospitality
- Culture
- EVS
- Featured Articles
- General Management
- Human Resources
- Imaging
- Inclusion and Belonging
- Information Technology
- Mentorship
- Nursing
- Operations
- Patient and Customer Experience
- Pharmacy
- Rehabilitation Services
- Revenue Cycle
- Social Services
- Students and Internships
- Veterans
- Wellness & Benefits
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019

Northwell Health remembers and spreads the light of our fallen heroes due to the COVID-19 pandemic
This March marked one year since Northwell treated the first case of COVID-19. While it has been a challenging year for all of us, the perseverance of our frontline heroes, the power of science, and the hope of ongoing vaccinations and innovative treatment plans brings us comfort for the path ahead.
The most difficult challenge has been coping with the grief associated with the loss of our colleagues, friends, family members and those in our communities. From March 9 to March 14, Northwell held remembrance activities to “spread the light” for our fallen team members and those who we have lost due to COVID-19. New York City – the epicenter of this pandemic – has also declared Sunday, March 14, as a Day of Remembrance to honor everyone we’ve lost.
To spread the light throughout our remembrance week, team members were encouraged to wear blue in memory of those who worked at Northwell and as a show of solidarity for our Northwell community. On site, our chaplains hosted moments of silence and remembrance circles to help our team members find meaning, hope, connection and comfort through togetherness regardless of religious affiliation. Spread the light activities were also available at our facilities, allowing team members to reflect by writing messages on remembrance boards, prayer cards, and lighting luminary bags to symbolize fallen team members.
Team members and their families also continued to spread the light in our communities over the past week as they organized light parades in their neighborhoods, created luminary bags and took a moment to pause to reflect with their loved ones.
During our remembrance week, Northwell also held an organization-wide Town Hall featuring our President and CEO, Michael Dowling, and other senior leaders, to connect our 75,000 team members and speak about the strength and sacrifice of our healthcare heroes. In addition to honoring those we have lost, it also recognized the efforts and unwavering dedication of our team members throughout the pandemic. From March 12 to March 14, our corporate headquarters in New Hyde Park, New York was illuminated in blue to honor our fallen team members and recognize the enduring courage and spirit of our Northwell community.

Throughout these challenging times, Northwell has also supported our team members by expanding benefits, offering prayer groups and providing well-being resources from our Team Lavender, a program at Northwell that provides staff with an opportunity for timely emotional, spiritual and physical support. These resources, such as Tranquility Tents, which offered areas of respite for our hospital workers during their shifts, and opportunities for 1:1 counseling through our Employee Assistance Program, have allowed for us to care for our team members as they delivered care to our communities. A 24/7, free and confidential, emotional support call center for all team members and their families also provided emotional well-being experts to answer their questions, provide additional resources, or just listen.
At Northwell Health, we will continue to battle this pandemic, look forward to brighter days, and support our team members.
We will always remember our brave fallen team members and their families. Join us as we spread the light.
Share this entry
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Recent Posts
- Explore two different career paths beginning as a nurse extern at Northwell Health.
- Mentorship, desired career growth, and making a difference: Meet Christopher, emergency department registered nurse
- Explore career paths in pharmacy at Northwell Health.
- From quality to operations: Discover Shivani’s career journey in labs
- Discover Tyler’s career journey in facilities and support services at Northwell Health
Categories
- Academia and Research
- Administrative Support
- Advance Clinical Providers
- Business
- Career Advice
- Career Paths
- Clinical Care
- Clinical Laboratory Science
- Clinical Support
- Culinary and Hospitality
- Culture
- EVS
- Featured Articles
- General Management
- Human Resources
- Imaging
- Inclusion and Belonging
- Information Technology
- Mentorship
- Nursing
- Operations
- Patient and Customer Experience
- Pharmacy
- Rehabilitation Services
- Revenue Cycle
- Social Services
- Students and Internships
- Veterans
- Wellness & Benefits
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019

Why our Phlebotomists love working at Northwell Health
Phlebotomists at Northwell Health play an important role by collecting blood samples from our patients. These blood samples can help identify a patient’s diagnosis and ultimately help doctors create a treatment plan for them. In February we are celebrating National Phlebotomists Recognition Week and we are proud to recognize the hard work and compassionate care that our phlebotomists deliver every day.
Meet some of our team members and learn why they love being a phlebotomist at Northwell:
 Luz Puig, Phlebotomist, Glen Cove Hospital
Luz Puig, Phlebotomist, Glen Cove Hospital
“My favorite thing about being a phlebotomist at Northwell is meeting patients and learning from their life experiences. I truly enjoy when they share their stories and I have a desire to make them feel comfortable and loved. During these hard times of COVID, my heart breaks to know many of the patients are alone during this process. I believe my role plays an important part in the healing of each patient as it is the start of a treatment for our community members.”
 Glenna McKenzie, Phlebotomist, Syosset Hospital
Glenna McKenzie, Phlebotomist, Syosset Hospital
“I have been a phlebotomist at Syosset Hospital for 35 years. I love being with our patients and doing my best to get their blood drawn quickly and painlessly. I love interacting with them and being able to get to know them. We understand that being ill and being in the hospital is not a high point for our patients, so I try my very best to make our patients feel better about their experience at our hospital.”
 Michelle Lyn Sambajon, Lead Phlebotomist, Northwell Health Labs
Michelle Lyn Sambajon, Lead Phlebotomist, Northwell Health Labs
“I oversee the COVID collection site for pre-procedure and pre-surgical testing. My favorite thing about working as a phlebotomist is that I enjoy being out there and helping people from their COVID test to bloodwork. Being a Phlebotomist is a rewarding opportunity to give back and help the community. It is the best feeling knowing that you’re one of the frontline team members to become a part of a person’s diagnostic treatment.”
 Amanda Salerno, Mobile Phlebotomy, Northwell Health Labs and LabFly
Amanda Salerno, Mobile Phlebotomy, Northwell Health Labs and LabFly
“I provide mobile services to patients to their personal residence for bloodwork and COVID swabs. The best part of my job is making people laugh and providing compassionate care. Anything to make someone’s heart feel a little lighter when I leave makes me happy. I go into every home the same, a smile, laughter, enlightenment when needed, compassion and with comfort in the experience I provide for them. A little goes a long way.”
 Maria L. Pizarro, Phlebotomist, Glen Cove Hospital
Maria L. Pizarro, Phlebotomist, Glen Cove Hospital
“I’ve worked at Glen Cove Hospital for 14 years as a phlebotomist. My job consists of drawing blood samples from in-patients. Patients are my priority and I really love what I do for the organization and working with my team.”
Discover a career well cared for as a phlebotomist at Northwell Health. Apply today!
Share this entry
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Recent Posts
- Explore two different career paths beginning as a nurse extern at Northwell Health.
- Mentorship, desired career growth, and making a difference: Meet Christopher, emergency department registered nurse
- Explore career paths in pharmacy at Northwell Health.
- From quality to operations: Discover Shivani’s career journey in labs
- Discover Tyler’s career journey in facilities and support services at Northwell Health
Categories
- Academia and Research
- Administrative Support
- Advance Clinical Providers
- Business
- Career Advice
- Career Paths
- Clinical Care
- Clinical Laboratory Science
- Clinical Support
- Culinary and Hospitality
- Culture
- EVS
- Featured Articles
- General Management
- Human Resources
- Imaging
- Inclusion and Belonging
- Information Technology
- Mentorship
- Nursing
- Operations
- Patient and Customer Experience
- Pharmacy
- Rehabilitation Services
- Revenue Cycle
- Social Services
- Students and Internships
- Veterans
- Wellness & Benefits
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019

Cardiovascular professionals at Northwell Health never miss a beat
Cardiovascular professionals at Northwell Health work diligently every day to keep our patients’ hearts healthy and strong. Whether they are technologists, EKG or monitor technicians, supervisors, registered nurses or another role, their hard work provides outstanding patient care that creates a positive impact in our community.
Meet some of our cardiovascular professionals:
 Maryann Colacino Boland, MSN, CNL, CCRN, CVRN, Registered Nurse, Cardiac Catheterization Lab, Huntington Hospital
Maryann Colacino Boland, MSN, CNL, CCRN, CVRN, Registered Nurse, Cardiac Catheterization Lab, Huntington Hospital
As a nurse in a Cath Lab, Maryann assists in performing diagnostic and interventional procedures through continuous patient monitoring, and administration of medications, and patient education. “My absolute favorite aspect of working as a cardiovascular professional at Northwell is how we are as a team,” says Maryann. “We are cohesive, committed to one purpose with a bond that enables us to always optimize our patient outcomes. In addition, we serve our community by providing emergency care 24 hours a day, to prevent life-changing, long-lasting heart disease.”
 Suvada Louthan, RN, CV-BC, Cardiac Catheterization Lab and Interventional Recovery Room, Long Island Jewish Medical Center
Suvada Louthan, RN, CV-BC, Cardiac Catheterization Lab and Interventional Recovery Room, Long Island Jewish Medical Center
Suvada has grown into her role as a registered nurse in both the Cath Lab and the Recovery Suite for eight and a half years at Long Island Jewish Medical Center. In her role, she works in the lab for scheduled and emergent procedures and works in recovery for the pre- and post-patient experience. “Working in the lab can be very exciting,” says Suvada. “Professionally, there is instant gratification when we are in the lab, a vessel is opened, and the patient is no longer having severe chest pain. I am always learning and growing as a professional. It is so rewarding to contribute to the health and wellness of our patients both acutely in the lab and by teaching in the recovery room.”
 Michael Kleinschmidt, Supervisor, Cardiac Services, North Shore University Hospital
Michael Kleinschmidt, Supervisor, Cardiac Services, North Shore University Hospital
As a supervisor in Cardiac Services, Michael’s role consists of the day-to-day operation and staffing of the technologists in the Cath Lab, along with scheduling, training, and maintaining equipment quality. “My favorite thing about working as a cardiovascular professional is being able to help people and make a difference in their lives,” says Michael. “Working in healthcare can be one of the most rewarding career choices there is. I consider myself very fortunate to work in a field that is always changing and growing with new technologies, capabilities and ideas.” Michael feels the impact of cardiovascular professionals on the community is indescribable. “The service we provide to the community is second to none. Not only do we help during their procedure, but we can often help post procedure.”
 Leslie Pierre, Lead Invasive Cardiovascular Technologist, Adult Cardiac Cath Lab, Long Island Jewish Medical Center
Leslie Pierre, Lead Invasive Cardiovascular Technologist, Adult Cardiac Cath Lab, Long Island Jewish Medical Center
As an invasive cardiovascular technologist, Leslie helps greet patients, set them up in the room and explain procedures. His role includes operating, maintaining, and troubleshooting a variety of diagnostic and invasive equipment. Cardiovascular technologists are tasked with maintaining a sterile field while preparing the table and equipment before and during procedures. “I feel the work we do in the Cath Lab can change our patients’ outlook on their health,” says Leslie. “We have seen patients take that mindset back to their family and friends and become the foundation for them to want to be aware of their cardiac health as well.”
 Kathi Augeri, Invasive Cardiovascular Technologist (CVT), Huntington Hospital
Kathi Augeri, Invasive Cardiovascular Technologist (CVT), Huntington Hospital
Working as an invasive cardiovascular technologist in the Cath Lab, Kathi works closely with physicians to examine and treat patients with cardiac diseases. She circulates, supports, and assists all aspects of invasive cardiology. “My favorite thing about working as a CVT is being a part of a talented team of individuals who can literally fix a broken heart. The satisfaction that comes along with helping someone get through a nerve-wracking experience is immeasurable,” says Kathi.
 Patricia Soriano, DNP, RN, MSN, APRN-BC, Manager, Patient Care, Cardiac Cath Lab, Northern Westchester Hospital
Patricia Soriano, DNP, RN, MSN, APRN-BC, Manager, Patient Care, Cardiac Cath Lab, Northern Westchester Hospital
Recently opening in September 2020, the Cardiac Cath/EP Lab in Northern Westchester Hospital is a great addition to Northwell. Patricia was initially tasked with opening the lab and developing all aspects related to operations. “The impact on our community has been significant in that our patients can now obtain this care closer to home,” says Patricia. “Additionally, with the implementation of our STEMI program, they can receive emergent treatment at their doorstep, saving time and cardiac muscle.” Patricia explained that her team’s favorite thing about working as a cardiovascular professional is the ability to deliver quality cardiac care utilizing advanced technology to patients and achieving great outcomes.
Share this entry
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Recent Posts
- Explore two different career paths beginning as a nurse extern at Northwell Health.
- Mentorship, desired career growth, and making a difference: Meet Christopher, emergency department registered nurse
- Explore career paths in pharmacy at Northwell Health.
- From quality to operations: Discover Shivani’s career journey in labs
- Discover Tyler’s career journey in facilities and support services at Northwell Health
Categories
- Academia and Research
- Administrative Support
- Advance Clinical Providers
- Business
- Career Advice
- Career Paths
- Clinical Care
- Clinical Laboratory Science
- Clinical Support
- Culinary and Hospitality
- Culture
- EVS
- Featured Articles
- General Management
- Human Resources
- Imaging
- Inclusion and Belonging
- Information Technology
- Mentorship
- Nursing
- Operations
- Patient and Customer Experience
- Pharmacy
- Rehabilitation Services
- Revenue Cycle
- Social Services
- Students and Internships
- Veterans
- Wellness & Benefits
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019

Continuing to serve as a care coordinator at Northwell’s Military Liaison Services
Before Donald (DJ) St.Clair, LMSW, started his career at Northwell Health, he first served as a Corporal in the US Marine Corps.
It was after his return from service while transitioning to a civilian career, that DJ first began to think about entering the healthcare industry. “Health care is a great opportunity for any veterans who are exiting the service as it will continue to give you a sense of purpose,” says DJ. “There is a sense of accomplishment because we are able to give back to the very community we served during our time in the military.”
With the encouragement and help of a social worker in the Office of Veterans Affairs, DJ continued his education to become a Licensed Master Social Worker to pursue a goal of being able to help veterans and their families. With his help, DJ was able to obtain benefits he didn’t know he had access to –something he’s able to pay forward in his new role as care coordinator within Northwell’s Military Liaison Services.
Transitioning from his role as a social worker at Long Island Jewish Medical Center, DJ is now in a unique position to combine his clinical experience and time in the military to provide support to other veterans. As care coordinator, DJ works to help service members, veterans, and their families access Northwell’s healthcare and community services, as well as assists them with connecting with local resources for additional support. It is the exact kind of role he hoped for when he started a career in mental health.
“Physical and mental health are very important in the well-being of everyone, but especially the veteran population,” says DJ. “There are a great number of benefits that the veteran population might not know about and I’m able to connect them to these important resources. I’m happy for the opportunity to give back to my brothers and sisters.”
Along with offering peer-to-peer guidance, DJ takes pride in being able to connect veterans to things such as service-connected disability benefits, education benefits, and a support system of organizations that are willing to help veterans transition back into the civilian world, such as Northwell Health.
And being a former veteran himself, DJ knows firsthand what it’s like to be in their position as they return home or to civilian life. It makes him uniquely qualified to connect with those who need it and to help them figure out their next steps.
“It can be a challenge to work through the common stigma around veterans that reaching for help means you are weak,” explains DJ. “In my role, I’m able to create a bond with them in a short time and explain that this assistance isn’t much different than being together in the military. The same way we rely on each other while in the service to have each other’s backs, they can rely on me here.”
Make the transition to a civilian career with Northwell Health. Learn more about our commitment to veterans.
Share this entry
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Recent Posts
- Explore two different career paths beginning as a nurse extern at Northwell Health.
- Mentorship, desired career growth, and making a difference: Meet Christopher, emergency department registered nurse
- Explore career paths in pharmacy at Northwell Health.
- From quality to operations: Discover Shivani’s career journey in labs
- Discover Tyler’s career journey in facilities and support services at Northwell Health
Categories
- Academia and Research
- Administrative Support
- Advance Clinical Providers
- Business
- Career Advice
- Career Paths
- Clinical Care
- Clinical Laboratory Science
- Clinical Support
- Culinary and Hospitality
- Culture
- EVS
- Featured Articles
- General Management
- Human Resources
- Imaging
- Inclusion and Belonging
- Information Technology
- Mentorship
- Nursing
- Operations
- Patient and Customer Experience
- Pharmacy
- Rehabilitation Services
- Revenue Cycle
- Social Services
- Students and Internships
- Veterans
- Wellness & Benefits
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019

Making the transition from clinical care to healthcare administration
Christian Jocelyn always knew he wanted to work in the healthcare industry so he could help others. He was uncertain which career path to take, so he became an emergency medical technician (EMT) after college, which provided him with his first healthcare career opportunity delivering frontline care. His career journey at Northwell over the years brought Christian to his current role as director of operations in the Department of Neurosurgery at North Shore University Hospital (NSUH).
A few years after starting his career journey as an EMT, Christian became a paramedic and began to get involved in performance improvement projects. These projects not only helped leadership realize Christian’s potential and that lead him to be promoted to paramedic supervisor. This also helped Christian discover where he wanted his Northwell career to go.
“In my role as a supervisor, I was responsible for the day-to-day field operations for one of the largest hospital-based EMS departments in the country. I had the opportunity to view the health system through a unique lens,” says Christian. “I came to understand the importance of caring for patients across all care settings and the strength of an integrated healthcare delivery system. This experience motivated me to go back to school and obtain my Masters in Health Administration and to begin the transition from clinician to administrator.”
While working toward his master’s degree, Christian transitioned out of EMS into a role as a manger of Financial and Operations Management at NSUH. It was this administrative foundation along with his education that enabled Christian to develop the skills he needed for his current role as director.
At Northwell, Christian has been able to build a rewarding career that utilizes his skills on the frontline to impact patient care through operations. Christian enjoys being able to take his experience and understanding of care outside of the hospital into designing programs within the hospitals. It is an opportunity he feels he was able to reach thanks in part to the mentors who supported his transition from clinical care to the administrative side of healthcare by removing barriers and helping him tap into his potential.
“One of the most important factors in my growth at Northwell has been my good fortune to have excellent mentors and sponsors along the way,” says Christian. “These individuals invested time, effort, and energy in me. They have set the example of what it means to be a leader and have provided the foundation I continue to build my career on. I would not be in the role or the person I am now without the expectational guidance and support by my mentors at Northwell.”
And for those looking to make a similar transition as Christian, he offers the advice of focusing on developing meaningful relationships in the organization and to not be afraid of taking risks. “Make it a point to collaborate with folks in other departments, step outside of your comfort zone and learn about a part of the organization that is unfamiliar to you,” he advises. “The beauty of Northwell is that we touch the entire continuum of care and with that comes an unparalleled learning opportunity.”
Discover a career well cared for at Northwell Health. Apply today!
Share this entry
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Recent Posts
- Explore two different career paths beginning as a nurse extern at Northwell Health.
- Mentorship, desired career growth, and making a difference: Meet Christopher, emergency department registered nurse
- Explore career paths in pharmacy at Northwell Health.
- From quality to operations: Discover Shivani’s career journey in labs
- Discover Tyler’s career journey in facilities and support services at Northwell Health
Categories
- Academia and Research
- Administrative Support
- Advance Clinical Providers
- Business
- Career Advice
- Career Paths
- Clinical Care
- Clinical Laboratory Science
- Clinical Support
- Culinary and Hospitality
- Culture
- EVS
- Featured Articles
- General Management
- Human Resources
- Imaging
- Inclusion and Belonging
- Information Technology
- Mentorship
- Nursing
- Operations
- Patient and Customer Experience
- Pharmacy
- Rehabilitation Services
- Revenue Cycle
- Social Services
- Students and Internships
- Veterans
- Wellness & Benefits
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019

Meet respiratory therapist and healthcare hero, Emily Shi
The dedication of our respiratory care team at Northwell Health is indescribable, especially during the unprecedented times of COVID-19. Our respiratory therapists deliver vital care through their hard work, teamwork and compassion. This week we celebrate Respiratory Therapist Appreciation Week and recognize our extraordinary team members.
Meet Yang (Emily) Shi, assistant director of Respiratory Therapy at North Shore University Hospital (NSUH). Emily has grown in her career at Northwell since she started as a Respiratory Therapist in 2006 on the NICU unit at NSUH. Specializing in neonatal and adult critical care, Emily has developed a skillset that lets her explore many career opportunities and advance her knowledge as a respiratory therapist.
In her current role, Emily oversees the day-to-day operations of the Respiratory Therapy department which includes team management, projects and patient care. To further her education and management skills, she is currently pursuing her MBA in Management and Leadership with the assistance of the Northwell’s tuition reimbursement program.
Respiratory therapists have always been a vital part of the healthcare system, but when COVID-19 peaked the need for respiratory team members grew rapidly. During this time respiratory therapists worked tirelessly to save their patients’ lives and Emily and her team had to rethink the way they cared for their patients on ventilators, prioritize their resources and learn how to keep their patients and colleagues safe.
“It has been stressful yet rewarding to work as a respiratory therapist throughout the COVID-19 pandemic,” says Emily. “Nothing makes me prouder than seeing a patient being liberated from ventilator or oxygen support and seeing them go home to their loved ones. I am proud to work at Northwell Health because it is an organization that provides quality, innovative care and is invested in the well-being of their communities and team members.”
Thank you to all of Northwell’s respiratory therapy healthcare heroes today and every day. Join the respiratory therapist heroes at Northwell Health.
Share this entry
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Recent Posts
- Explore two different career paths beginning as a nurse extern at Northwell Health.
- Mentorship, desired career growth, and making a difference: Meet Christopher, emergency department registered nurse
- Explore career paths in pharmacy at Northwell Health.
- From quality to operations: Discover Shivani’s career journey in labs
- Discover Tyler’s career journey in facilities and support services at Northwell Health
Categories
- Academia and Research
- Administrative Support
- Advance Clinical Providers
- Business
- Career Advice
- Career Paths
- Clinical Care
- Clinical Laboratory Science
- Clinical Support
- Culinary and Hospitality
- Culture
- EVS
- Featured Articles
- General Management
- Human Resources
- Imaging
- Inclusion and Belonging
- Information Technology
- Mentorship
- Nursing
- Operations
- Patient and Customer Experience
- Pharmacy
- Rehabilitation Services
- Revenue Cycle
- Social Services
- Students and Internships
- Veterans
- Wellness & Benefits
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
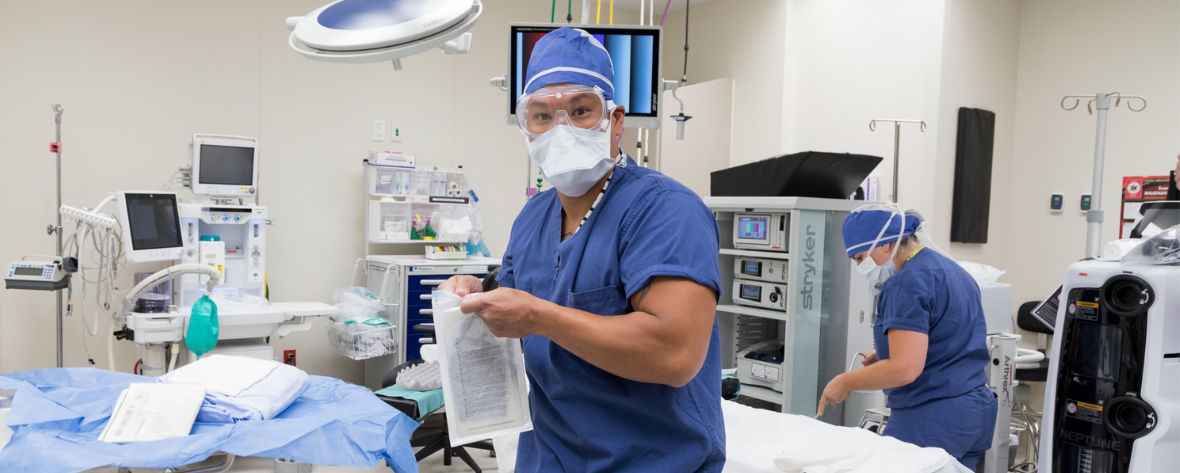
The rewarding work of a surgical technologist at Northwell Health
The work of surgical technologists in our operating rooms is a vital part of the perioperative services at Northwell Health. Working alongside our surgeons and nurses, surgical technologists who prepare our operating rooms, arrange equipment, and help team members during surgeries. This Surgical Technologist Appreciation Week and every day, we celebrate our team members.
Meet Jason Dizon, a surgical technologist at Plainview Hospital who is just one of these integral team members keeping our operating rooms running smoothly and ensuring patient safety every step of the way.
Jason has as a surgical technologist at Plainview Hospital for almost five years, but his love for the operating room has him planning to stay until he retires. Working in surgery means his job is never mundane, and each case brings him a new opportunity to learn. Innovative surgeries in our hospitals also provides the chance for Jason to grow his skills as he helps prepare the OR with cutting-edge technology and works as a member of the surgical team.
At Plainview Hospital, Jason focuses mostly on orthopedic cases, such as total joint replacements or spine cases, but has been able to experience work on a variety of specialties. “I have grown a lot working at Plainview Hospital,” says Jason. “We have great leadership that supports us and it’s a great place to work because we are able to learn from a diverse group of team members.”
And within his role, Jason also develops his skillset by helping to teach others. “Teaching and speaking with surgical technologist students and nursing students helps me improve my communication skills,” says Jason. “It’s taught me to always use patience and understanding as students grow in their skills.” Working with the enthusiastic students and helping to teach them about working in perioperative services is one of Jason’s favorite parts of his job. With perioperative services not often focused on in schools, Jason is there for what is often the first look these students get into an operating room. It’s an eye-opening experience he values being a part of.
But it’s not the only responsibility that makes Jason so passionate about what he does. “I love my job. I love science and health, and as a surgical technologist, I’m able to learn every day about the human body and how it functions. To see firsthand how we heal patients and take care of them is very rewarding.”
Interested in a surgical technologist career at Northwell? Apply today!
Share this entry
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Recent Posts
- Explore two different career paths beginning as a nurse extern at Northwell Health.
- Mentorship, desired career growth, and making a difference: Meet Christopher, emergency department registered nurse
- Explore career paths in pharmacy at Northwell Health.
- From quality to operations: Discover Shivani’s career journey in labs
- Discover Tyler’s career journey in facilities and support services at Northwell Health
Categories
- Academia and Research
- Administrative Support
- Advance Clinical Providers
- Business
- Career Advice
- Career Paths
- Clinical Care
- Clinical Laboratory Science
- Clinical Support
- Culinary and Hospitality
- Culture
- EVS
- Featured Articles
- General Management
- Human Resources
- Imaging
- Inclusion and Belonging
- Information Technology
- Mentorship
- Nursing
- Operations
- Patient and Customer Experience
- Pharmacy
- Rehabilitation Services
- Revenue Cycle
- Social Services
- Students and Internships
- Veterans
- Wellness & Benefits
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019

Appointment With: Abdo Nahmod, AVP, CEMS Operations
Northwell Health’s Center for Emergency Medical Services (CEMS) team members often provide the first line of care to patients in the neighborhoods and communities we serve. Abdo Nahmod, assistant vice president of CEMS Operations, has helped to lead the team through both rewarding and challenging times since starting five years ago.
We sat down with Abdo to talk about CEMS initiatives on the horizon and the exciting job opportunities within the team:
How has CEMS grown over the past year?
CEMS has been progressively growing in providing quality pre-hospital care to more of the communities we serve. Over the past year we have expanded our services in Nassau and Suffolk counties and New York City, as well as added a Northwell Health Centralized Transfer Center to manage inter-facility patient transfers through the CEMS Communication Center.
We have also collaborated with Northwell’s Center for Learning and Innovation (CLI) to provide our team members with paramedic training opportunities. This is an investment in our team members, as we promote from within emergency medical technicians to paramedics, providing career opportunities for advancement and retention. This past year we also supported many team members who choose to further their clinical and post-graduate education with Northwell’s tuition reimbursement program.
How has the work of CEMS been vital to our organizations and communities during the COVID-19 pandemic?
During COVID-19, CEMS has provided emergency medical care throughout the seven counties we serve. We have seen a surge in EMS call volume for critically ill patients, providing life-saving treatments and transportation to many hospitals. CEMS had transferred over 900 COVID -19 patients throughout Northwell for continued care in March and April. We are also working with Northern Westchester Hospital’s community services team to be part of the COVID -19 testing at faith-based venues, and we will be collaborating with the FDNY for 311 and 911 telemedicine services in the near future.
What exciting initiatives are on the horizon for CEMS?
We are looking forward to the expansion of our Centralized Transfer Center, collaborating with FDNY in New York City for 311 & 911 Telemedicine services. CEMS continues to be a highly engaged workforce with a culture of teamwork and recognition. We view every challenge as an opportunity, and seek feedback while relentlessly pursuing what is best. We prize curiosity, creativity and innovation.
What careers exist within the CEMS team?
We have over a dozen job titles within CEMS such as, emergency medical technicians, paramedics, communications specialists, ambulance supply associates, flight paramedics, flight nurses, ambulance record associates, staffing schedule associates and various supervisory and leadership titles.
Our team continues to be a highly engaged workforce with a culture of teamwork and recognition. We view every challenge as an opportunity, and seek feedback while relentlessly pursuing what is best. We prize curiosity, creativity and innovation. The expectation is everyone learns, develops and becomes better. Our culture promotes self-development, ongoing education and career growth and advancement. Our reputation is everyone’s responsibility.
What career advice do you have for those looking to get into Emergency Medicine Services (EMS)?
My best advice is to volunteer in EMS in your community and see if this is something you enjoy enough to pursue as a career. EMS may be a gateway to opportunities within healthcare to other clinical and non-clinical opportunities.
Share this entry
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Recent Posts
- Explore two different career paths beginning as a nurse extern at Northwell Health.
- Mentorship, desired career growth, and making a difference: Meet Christopher, emergency department registered nurse
- Explore career paths in pharmacy at Northwell Health.
- From quality to operations: Discover Shivani’s career journey in labs
- Discover Tyler’s career journey in facilities and support services at Northwell Health
Categories
- Academia and Research
- Administrative Support
- Advance Clinical Providers
- Business
- Career Advice
- Career Paths
- Clinical Care
- Clinical Laboratory Science
- Clinical Support
- Culinary and Hospitality
- Culture
- EVS
- Featured Articles
- General Management
- Human Resources
- Imaging
- Inclusion and Belonging
- Information Technology
- Mentorship
- Nursing
- Operations
- Patient and Customer Experience
- Pharmacy
- Rehabilitation Services
- Revenue Cycle
- Social Services
- Students and Internships
- Veterans
- Wellness & Benefits
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
Contact us
If you are an individual with a disability requesting an accommodation for the application process, please click the contact us link above to request assistance.
Learn more about our hiring experience.
Read answers to common questions about the application process.
© 2026 - Northwell Health
If you are an individual with a disability requesting an accommodation for the application process, please click the contact us link above to request assistance.
Learn more about our hiring experience.
Read answers to common questions about the application process.
© 2026 - Northwell Health
It is Northwell Health’s policy to provide equal employment opportunity and treat all applicants and employees equally regardless of age, race, creed/religion, color, national origin, immigration status, or citizenship status, military or veteran status, sexual orientation, sex/gender, gender identity, gender expression, height, weight, disability, pregnancy, genetic information or genetic predisposition or carrier status, marital or familial status, partnership status, victim of domestic violence, their or their dependent’s sexual or other reproductive health decisions, or other characteristics protected by applicable law.
Northwell Health reserves the right to amend all terms of employment.









