Archive for month: August, 2020

Day in the life: Sourcing specialist in Talent Acquisition
Meet Bridget Hanley, sourcing specialist in Talent Acquisition (TA) at Northwell Health. Focusing on perioperative, labor and delivery, and emergency nursing, among other specialties, Bridget identifies top talent for much needed roles across the organization using a variety of sourcing strategies and recruitment tools. As one of many roles in Human Resources, sourcing specialists are focused on finding the best talent to join our organization to deliver the best level of care to our patients.
Bridget, like many of our non-clinical team members, had to adapt to a new way of working remotely due to COVID-19 to ensure the well-being of our team members and their families. As one of Northwell’s department wellness liaisons, Bridget played a particularly important role since the beginning of the pandemic to ensure wellness was top of mind for all of our talent acquisition team members during this challenging time by providing tips, strategies and opportunities to stay healthy both physically and mentally while working from home in this new environment.
Follow a day in her life working remotely as a sourcing specialist:

Starting her day with morning stretches, Bridget then fuels up with a smoothie and coffee. She reads the news, checks professional social media accounts , and keeps an eye out for any recent healthcare trends—all to help her better connect with candidates for careers at Northwell. “One reason I enjoy working remotely is more ‘me’ time in the morning. I can start my day with different healthy habits, which is a welcome change from the daily commute,” says Bridget.

As a member of Talent Acquisition, Bridget uses different tools and strategies to find potential candidates and engage with them.. Beyond available shifts and locations, Bridget helps educate them about all the benefits and resources that come along with working within our organization, a Fortune 100 Best Places to Work. Here she is speaking with a nurse about one of Northwell’s major perks – tuition reimbursement!

As a Northwell wellness liaison, Bridget shares daily emails with the team highlighting wellness programs, healthy recipes, exercise tips and more. Taking a five-minute break, she practices a daily stretch recommended by our Employee Wellness team in collaboration with the myHealthyBody app that our team members have access to use. “Our department can be very fast-paced and I love providing tips and resources to help us remember to focus on our own wellbeing.”

Beyond sourcing, Bridget partners with other teams across Northwell to help educate candidates on best hiring practices. Volunteering for Northwell’s new Career Development Certificate Program, Bridget presented on how to build your personal brand, including networking and social media tips. “Over 400 students and professionals attended the live session, and I was impressed with the engagement and questions they presented during the Q&A session. I’ve already had someone thank me on LinkedIn for helping them be prepared for their Northwell interview!”

Presentation over, it’s back to sourcing. Enjoying the warm weather, Bridget steps outside for a few scheduled calls with interested candidates. What is Bridget’s favorite part of her job? “I enjoy meeting and speaking with new people and helping them in their career. Every candidate I talk to has their own story and teaches me something new. Sharing the opportunities Northwell has and figuring out how the candidate will best add value to our organization is exciting. I feel lucky to play a part in their journey.”

As Bridget’s role has expanded, so have her responsibilities. In addition to sourcing, her afternoon often involves testing new Human Resource systems, piloting sourcing tools and recruitment platforms, and enabling for an improved candidate and recruiter experience through new technology. Working with recruiters across the health system from Westchester to Riverhead also means weekly phone calls and team meetings are necessary to stay updated on candidates, staffing requirements, and anticipating hiring needs within Northwell.

Work day over, Bridget embraces Northwell’s commitment to wellness by engaging in physical activity. Running has the added benefit of helping her prepare for Northwell’s next Walk To.. step challenge where Northwell teams compete to reach a step goal to win prizes.
Find a job that’s a perfect fit for your lifestyle at Northwell Health. Get moving and apply today.
Share this entry
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Recent Posts
- Discover Kenneth’s career journey to a physical therapist at Northwell Health
- Explore two different career paths beginning as a nurse extern at Northwell Health.
- Mentorship, desired career growth, and making a difference: Meet Christopher, emergency department registered nurse
- Explore career paths in pharmacy at Northwell Health.
- From quality to operations: Discover Shivani’s career journey in labs
Categories
- Academia and Research
- Administrative Support
- Advance Clinical Providers
- Business
- Career Advice
- Career Paths
- Clinical Care
- Clinical Laboratory Science
- Clinical Support
- Culinary and Hospitality
- Culture
- EVS
- Featured Articles
- General Management
- Human Resources
- Imaging
- Inclusion and Belonging
- Information Technology
- Mentorship
- Nursing
- Operations
- Patient and Customer Experience
- Pharmacy
- Rehabilitation Services
- Revenue Cycle
- Social Services
- Students and Internships
- Veterans
- Wellness & Benefits
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019

Appointment With: Abdo Nahmod, AVP, CEMS Operations
Northwell Health’s Center for Emergency Medical Services (CEMS) team members often provide the first line of care to patients in the neighborhoods and communities we serve. Abdo Nahmod, assistant vice president of CEMS Operations, has helped to lead the team through both rewarding and challenging times since starting five years ago.
We sat down with Abdo to talk about CEMS initiatives on the horizon and the exciting job opportunities within the team:
How has CEMS grown over the past year?
CEMS has been progressively growing in providing quality pre-hospital care to more of the communities we serve. Over the past year we have expanded our services in Nassau and Suffolk counties and New York City, as well as added a Northwell Health Centralized Transfer Center to manage inter-facility patient transfers through the CEMS Communication Center.
We have also collaborated with Northwell’s Center for Learning and Innovation (CLI) to provide our team members with paramedic training opportunities. This is an investment in our team members, as we promote from within emergency medical technicians to paramedics, providing career opportunities for advancement and retention. This past year we also supported many team members who choose to further their clinical and post-graduate education with Northwell’s tuition reimbursement program.
How has the work of CEMS been vital to our organizations and communities during the COVID-19 pandemic?
During COVID-19, CEMS has provided emergency medical care throughout the seven counties we serve. We have seen a surge in EMS call volume for critically ill patients, providing life-saving treatments and transportation to many hospitals. CEMS had transferred over 900 COVID -19 patients throughout Northwell for continued care in March and April. We are also working with Northern Westchester Hospital’s community services team to be part of the COVID -19 testing at faith-based venues, and we will be collaborating with the FDNY for 311 and 911 telemedicine services in the near future.
What exciting initiatives are on the horizon for CEMS?
We are looking forward to the expansion of our Centralized Transfer Center, collaborating with FDNY in New York City for 311 & 911 Telemedicine services. CEMS continues to be a highly engaged workforce with a culture of teamwork and recognition. We view every challenge as an opportunity, and seek feedback while relentlessly pursuing what is best. We prize curiosity, creativity and innovation.
What careers exist within the CEMS team?
We have over a dozen job titles within CEMS such as, emergency medical technicians, paramedics, communications specialists, ambulance supply associates, flight paramedics, flight nurses, ambulance record associates, staffing schedule associates and various supervisory and leadership titles.
Our team continues to be a highly engaged workforce with a culture of teamwork and recognition. We view every challenge as an opportunity, and seek feedback while relentlessly pursuing what is best. We prize curiosity, creativity and innovation. The expectation is everyone learns, develops and becomes better. Our culture promotes self-development, ongoing education and career growth and advancement. Our reputation is everyone’s responsibility.
What career advice do you have for those looking to get into Emergency Medicine Services (EMS)?
My best advice is to volunteer in EMS in your community and see if this is something you enjoy enough to pursue as a career. EMS may be a gateway to opportunities within healthcare to other clinical and non-clinical opportunities.
Share this entry
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Recent Posts
- Discover Kenneth’s career journey to a physical therapist at Northwell Health
- Explore two different career paths beginning as a nurse extern at Northwell Health.
- Mentorship, desired career growth, and making a difference: Meet Christopher, emergency department registered nurse
- Explore career paths in pharmacy at Northwell Health.
- From quality to operations: Discover Shivani’s career journey in labs
Categories
- Academia and Research
- Administrative Support
- Advance Clinical Providers
- Business
- Career Advice
- Career Paths
- Clinical Care
- Clinical Laboratory Science
- Clinical Support
- Culinary and Hospitality
- Culture
- EVS
- Featured Articles
- General Management
- Human Resources
- Imaging
- Inclusion and Belonging
- Information Technology
- Mentorship
- Nursing
- Operations
- Patient and Customer Experience
- Pharmacy
- Rehabilitation Services
- Revenue Cycle
- Social Services
- Students and Internships
- Veterans
- Wellness & Benefits
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019

Johanna Moustouka embraced the Northwell Heroes Challenge as she continues her wellness journey
When Johanna Moustouka started her career journey at Northwell Health 11 years ago she looked forward to a career as a nursing assistant and to developing her skills professionally. She never realized the impact that the organization would also have on her personal life, especially on her wellness journey. Today, Johanna is a wellness champion and liaison at Northwell and also at home, and she is a triathlete who is always striving to reach her professional and personal goals.
Starting out at Glen Cove Hospital in the Rehabilitation Unit and eventually transitioning to the Emergency Department at Huntington Hospital, Johanna has gained career experience caring for patients with different illnesses. Along her Northwell career journey, she also became more aware of her physical and mental wellbeing, realizing that by living a healthier lifestyle she could help provide better care for her patients. Northwell has helped Johanna achieve her wellness goals by offering a great environment for leading a healthy lifestyle.
“I have always loved the wellness awareness and initiatives that Northwell provides to their employees such as, the yearly walking challenges, the wellness app, and the many events that Northwell sponsors as additional motivation,” she says.
Being a Northwell wellness liaison, Johanna also shares her wellness experiences with her colleagues at Huntington Hospital. She encourages her teammates to exercise including three-minute workouts on their breaks and going for walks. She realized if she was healthy and strong, she would be able to provide better care for her patients and her family. She also wanted to teach her five kids good wellness habits and instill in them that you can do anything you set your mind to, but you must lead by example. And, Johanna did just that.
Leveraging Northwell’s benefits, Johanna was able to instill healthy habits such as clean eating, clean shopping, and being physically active. This helped her family to adapt a healthy lifestyle! Johanna explained that her kids enjoyed partaking in her journey as a triathlete and training for the half marathon. They have done multiple 5k runs, completed races, and they go to the gym together. “I absolutely love how on board they are with all of this because it’s keeping them healthy and it’s extra bonding time for us,” she says.
Johanna leads a very active life and understands the true meaning of dedication. “Being a triathlete or a runner requires a significant amount of determination and discipline. You have to be able to balance work, family time and training. That could mean doing an open water swim or run at 5:00 am before punching into work at 6:45 am or a late afternoon or evening bike ride or run before bed,” Johanna said.
While working in the Emergency Room Department during the COVID-19 pandemic, Johanna saw how hard her team members were working and wanted to give back to her fellow heroes. She decided to participate in the Northwell Heroes Challenge during the first weekend of August. This wellness Challenge allowed employees to get moving while raising money for the Northwell Heroes Caregiver Support Fund, which provides programs and services to team members in need of emotional, psychological or financial support and more.
Johanna is a Northwell hero who goes above and beyond for her patients, the organization, and her family. Northwell’s culture and wellness encourages our employees’ growth professionally and personally, and Johanna is Made for this.
Share this entry
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Recent Posts
- Discover Kenneth’s career journey to a physical therapist at Northwell Health
- Explore two different career paths beginning as a nurse extern at Northwell Health.
- Mentorship, desired career growth, and making a difference: Meet Christopher, emergency department registered nurse
- Explore career paths in pharmacy at Northwell Health.
- From quality to operations: Discover Shivani’s career journey in labs
Categories
- Academia and Research
- Administrative Support
- Advance Clinical Providers
- Business
- Career Advice
- Career Paths
- Clinical Care
- Clinical Laboratory Science
- Clinical Support
- Culinary and Hospitality
- Culture
- EVS
- Featured Articles
- General Management
- Human Resources
- Imaging
- Inclusion and Belonging
- Information Technology
- Mentorship
- Nursing
- Operations
- Patient and Customer Experience
- Pharmacy
- Rehabilitation Services
- Revenue Cycle
- Social Services
- Students and Internships
- Veterans
- Wellness & Benefits
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019

Phelps Hospital wins Northwell Health’s 2020 Chefs Challenge
Five Northwell Health hospitals recently competed in the 2020 Chefs Challenge at Glen Cove Hospital! Chefs, cooks and one certified dietitian worked together to prepare a healthy and delicious three course meal within 90 minutes. After presenting their wild sea bass appetizer, Long Island duck entrée, and strawberry dessert to our judges for tasting, Phelps Hospital was awarded first place in the competition. The Northern Westchester Hospital team came in second while the Huntington Hospital team placed third.
You’ve already met this year’s teams, now take a look at their delicious meals!
First Place: Phelps Hospital

Second Place: Northern Westchester Hospital

Third Place: Huntington Hospital

North Shore University Hospital

Southside Hospital

At Northwell, we believe food has the power to heal. Learn more about our culinary careers.
Share this entry
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Recent Posts
- Discover Kenneth’s career journey to a physical therapist at Northwell Health
- Explore two different career paths beginning as a nurse extern at Northwell Health.
- Mentorship, desired career growth, and making a difference: Meet Christopher, emergency department registered nurse
- Explore career paths in pharmacy at Northwell Health.
- From quality to operations: Discover Shivani’s career journey in labs
Categories
- Academia and Research
- Administrative Support
- Advance Clinical Providers
- Business
- Career Advice
- Career Paths
- Clinical Care
- Clinical Laboratory Science
- Clinical Support
- Culinary and Hospitality
- Culture
- EVS
- Featured Articles
- General Management
- Human Resources
- Imaging
- Inclusion and Belonging
- Information Technology
- Mentorship
- Nursing
- Operations
- Patient and Customer Experience
- Pharmacy
- Rehabilitation Services
- Revenue Cycle
- Social Services
- Students and Internships
- Veterans
- Wellness & Benefits
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
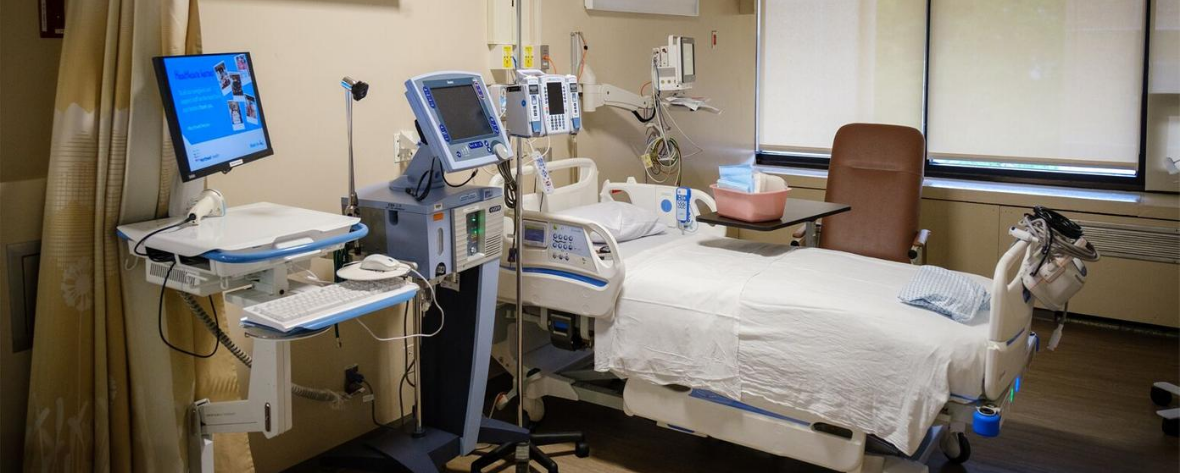
Delivering specialized respiratory care in a new unit at Northern Westchester Hospital
As the battle against COVID-19 continuously evolves, so does the care Northwell Health teams are delivering to our patients. With the shift to recovery, Northwell has opened two specialized, acute ventilator recovery units (AVRUT). The new unit at Northern Westchester Hospital (NWH) and its sister unit at Glen Cove Hospital will provide focused rehabilitation to patients recovering from COVID-19.
Physicians, nurses, respiratory therapists (RTs), dietitians and physical therapists (PTs) will all work together in these units for 24/7 care. Within these converted units, team members will have the specialized medical equipment and other essential items needed for the recovering intensive care patients who received tracheotomies in order to receive mechanical ventilator care.
Within these new units, respiratory therapists will play an essential role delivering around-the-clock ventilator and tracheotomy care. RTs will work alongside PTs to help their patients in need of ventilator weaning physical, occupational and speech therapy. The work of these team members helps wean patients off ventilators and helps this special patient population recover from their illness as they transition to a more traditional rehab facility.
This dedicated care has already seen success as patients are getting up and walking quicker than ever according to Pete Sequinot Jr., RRT, manager of Respiratory Care, Sleep Center and Pulmonary Rehab at NWH.
“Northwell Health is the best place for respiratory therapists to work,” says Pete. “At Northern Westchester Hospital, our average is 12 years of service. Northwell is always trying new things in respiratory care and administration truly listens to our ideas and concerns. Respiratory therapists come here and they feel like their voices are heard at all times.”
By creating these units for more specialized care, team members are not only helping patients recover but alleviating stress from Northwell’s ICUs. These new units mean patients can be transferred out of the ICU, allowed more critical care team members to return to their normal operating conditions.
The respiratory therapists and other AVRU team members continue to help patients recovering from COVID-19, providing regular consultation to asses recovery goals and next steps. Together they’re helping patients recover alongside our communities.
“At the end of the day, I would go into war with this team. They exceeded all expectations throughout the COVID-19 pandemic and showed that they are all team players. I am so proud of them and consider them family. If you want the best possible care for your loved ones, come here to Northwell and Northern Westchester Hospital.”
Are you Made for delivering respiratory care? Register for our Respiratory Therapist Virtual Interview Days to learn about full-time and part-time respiratory therapist opportunities.
Share this entry
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Recent Posts
- Discover Kenneth’s career journey to a physical therapist at Northwell Health
- Explore two different career paths beginning as a nurse extern at Northwell Health.
- Mentorship, desired career growth, and making a difference: Meet Christopher, emergency department registered nurse
- Explore career paths in pharmacy at Northwell Health.
- From quality to operations: Discover Shivani’s career journey in labs
Categories
- Academia and Research
- Administrative Support
- Advance Clinical Providers
- Business
- Career Advice
- Career Paths
- Clinical Care
- Clinical Laboratory Science
- Clinical Support
- Culinary and Hospitality
- Culture
- EVS
- Featured Articles
- General Management
- Human Resources
- Imaging
- Inclusion and Belonging
- Information Technology
- Mentorship
- Nursing
- Operations
- Patient and Customer Experience
- Pharmacy
- Rehabilitation Services
- Revenue Cycle
- Social Services
- Students and Internships
- Veterans
- Wellness & Benefits
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
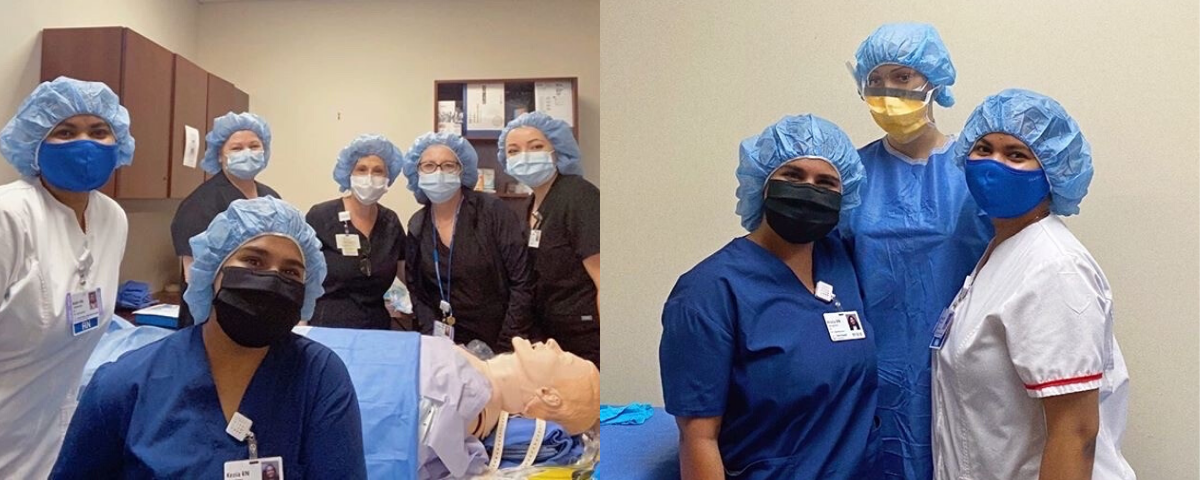
Meet the Truly Innovative Perioperative Fellowship team
Kezia Varughese, a registered nurse, was thrilled to get the call that she was accepted into the Perioperative Nurse Fellowship Program at North Shore University Hospital (NSUH), especially given her interest in learning more about working in an operating room.
Kezia felt a strong connection with the OR when she had the opportunity to shadow a nurse during surgery at nursing school. The patient expressed to Kezia that she was anxious about the procedure, even though her surgery was low risk. She tried to comfort the patient by talking about good memories and laughing about stories of her children. “She told me how she hadn’t laughed like this in a very long time, and how grateful she was that I was there for her during this vulnerable time,” says Kezia.
That was the moment Kezia realized how it takes a special kind of person and team to be with those who are admitted for surgery. She knew this was a great opportunity to expand her knowledge and nursing skills into the operating room.
The Perioperative Nursing Fellowship
Kezia began the fellowship program during the COVID pandemic. She was told by the educators how the fellowship was conducted before COVID which typically included lectures one day and the following day would be a “skills” day in the hospital. The skills day is where fellows simulate what they learned the previous day during their lectures.
Then due to the COVID-19 pandemic, an entirely different approach to the program had to be taken—an approach that required a setting outside of the hospital. This took some creative thinking and teamwork to simulate real-life patient care scenarios using a makeshift operating room.
“Despite all the stress and hardships COVID-19 created, our educators exemplified the true meaning of dedication, resilience, and perseverance,” says Kezia. “The constant desire to serve as a resource and attend to everyone’s needs, especially in such a troubling time, is one of the main factors that helped me feel comfortable in a not-so comfortable time.”
Support from Leadership
The support and collaboration among the leadership team and other team members during the program was extraordinary. Not only were the nurse educators welcoming, but they encouraged the team to communicate freely and offer feedback when needed. Most of Kezia’s trainings was conducted with Microsoft Teams and various in-person simulation days that included socially distanced groups of four who collaborated in a makeshift operating room. Despite the non-traditional approach, Kezia explained that the COVID pandemic did not affect their ability to be well prepared.
In fact, Kezia gained insight as to what it’s like to work in a fast-paced environment, develop critical thinking skills, organizational and interpersonal skills, and how to work with a team to deliver exceptional patient care. The most important concept Kezia learned was how to fully understand and provide the upmost quality of care for her patient, while ensuring the patient’s safety. “The compassion and advocacy my educators demonstrated for us illustrated the care that their patients receive. This was the most eye-opening and inspiring aspect of the Perioperative Fellowship,” Kezia says.
“An OR nursing career is one of the most rewarding careers,” says Kezia. She encourages new graduates and nurses to participate in the fellowship. “It allows one to develop the professional nursing skills that textbooks and nursing school could never teach.”
No matter what our team members are facing, their priority is to deliver compassionate care for our patients. Kezia and her team at NSUH exemplify Northwell’s value of Truly Innovative!
Are you Made for an opportunity like this?
The next step in your career is up to you! To learn more about being a part of our fellowship programs, click here.
Share this entry
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Recent Posts
- Discover Kenneth’s career journey to a physical therapist at Northwell Health
- Explore two different career paths beginning as a nurse extern at Northwell Health.
- Mentorship, desired career growth, and making a difference: Meet Christopher, emergency department registered nurse
- Explore career paths in pharmacy at Northwell Health.
- From quality to operations: Discover Shivani’s career journey in labs
Categories
- Academia and Research
- Administrative Support
- Advance Clinical Providers
- Business
- Career Advice
- Career Paths
- Clinical Care
- Clinical Laboratory Science
- Clinical Support
- Culinary and Hospitality
- Culture
- EVS
- Featured Articles
- General Management
- Human Resources
- Imaging
- Inclusion and Belonging
- Information Technology
- Mentorship
- Nursing
- Operations
- Patient and Customer Experience
- Pharmacy
- Rehabilitation Services
- Revenue Cycle
- Social Services
- Students and Internships
- Veterans
- Wellness & Benefits
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019

A humble hero of America’s COVID-19 response
Written by: Brian Donnelly
In one 29-hour period, a nurse practitioner assessed and treated some of the earliest COVID-19 patients in the US stuck aboard a cruise ship off the coast of California.
Bouncing back and forth in nautical step with the rough tide of the San Francisco coast, Bryan Lovejoy, DNP, 37, and his eight-person team passed under the Golden Gate Bridge; then the Bay Bridge in a small US Coast Guard patrol boat.
It was March 8, 2020.
“It was actually a nice little cruise when you get right down to it,” Mr. Lovejoy said, despite the sounds of seasickness surrounding him. “There were whales at one point, just kind of jumping around out there.”
Passing Alcatraz, the nurse practitioner at North Shore University Hospital (NSUH) — now farther than 3,000 miles from home — knew they were getting close to their destination — a 1,000-foot, 14-deck luxury cruise liner carrying 2,300 passengers and 1,100 crew members. The Grand Princess had been stuck 50 miles off the coast for days due to COVID-19 spreading rapidly among those onboard.
“I was kind of nervous about it. I saw the news,” he said. “The plan at the time was to try to keep this novel coronavirus out of the US as much as we could. Of course, we soon found out community spread was inevitable.”
The father of two and Smithtown, NY, resident is part of a 30-member disaster medical assistance team (DMAT). On behalf of the Department of Health and Human Services, DMAT responds to areas impacted by a health care crisis, like natural disasters, when local response capabilities are impaired.
In 2017 Mr. Lovejoy spent two weeks in both Houston and Puerto Rico in response to deadly hurricanes.
“You just don’t know what you’re going into entirely,” he said. “The situations are very dynamic.”
But, from March 8-9, an eight-person DMAT contingent faced a threat unlike any they had seen before.
“Our main objective was to identify how prevalent COVID-19 was on the ship before taking passengers off,” said Mr. Lovejoy, who joined DMAT in 2007. “Not many people had any experience with this virus yet, and definitely not on a cruise ship.”
Bryan Lovejoy treats a patient at North Shore University Hospital, where he is co-chair of the Collaborative Care Council for the advance care provider team.

Being prepared
Mr. Lovejoy’s coworkers at NSUH saw their first COVID-19 patient March 7, while he was heading out west to his next mission.
“Especially under the circumstances we are in during a crisis, it takes a leader like Mr. Lovejoy to put aside his personal priorities and become actively involved in a life-threatening mission like this,” said Susan Wirostek, nurse manager at NSUH.
There are two months each year during which a DMAT volunteer can be called into service, which is why Mr. Lovejoy keeps a bag packed with some basic necessities.
“You never really get used to it,” said Mr. Lovejoy’s wife, Dawn, 39. “Every situation is different. They’re all anxiety producing in their own way.”
The call for this latest mission came just before midnight on March 6. After spending a day with their kids, Julia, 9, and James, 5, he and Dawn were watching a movie — John Wick 2.
“Sometimes I have very limited notice,” he said, adding he still hasn’t seen the end of that movie. “I’m given my travel orders, I pack my bags and I’m out within a day going to wherever this is.”
Boarding the Grand Princess
Mr. Lovejoy was on a plane by 8 a.m. the next morning. Leaving his family, he said, is often the most difficult part of his work.
“This one definitely stood out as the worst,” Dawn added, “because as time progressed the virus got worse and worse here in New York. I was scared.”
With the Grand Princess in sight, the team of eight braved high swells and dangerous conditions to board a life raft sent to their US Coast Guard transport – the first of two “high consequence, zero margin transfers,” wrote Robert Kadlec, MD, assistant secretary for preparedness and response (ASPR), in a letter of commendation to Mr. Lovejoy.
“After safely boarding the Grand Princess, Mr. Lovejoy quickly demonstrated his clinical competencies and selfless focus on the mission as part of the HASTY rapid triage team, which executed near continuous operations for 29 hours, while wearing bio-containment equipment,” the high-ranking DHHS official wrote.
Jumping from the lifeboat onto the cruise ship ladder, Mr. Lovejoy’s team scaled the massive vessel, rung-by-rung.
“It’s big,” he admitted, quick to downplay the feet. “It didn’t take too long. I just remember thinking, ‘don’t look down and don’t let go.’”
Playing a crucial role
Starting near 7 p.m., Mr. Lovejoy worked through the night and into the next day, performing medical assessments and triage of more than 1,100 US citizens — breaking only for emergency rehydration. Mr. Kadlec wrote that their effort, “played a crucial role in the pre-positioning of critical medical assets, supporting personnel and operational planning by federal, state and local emergency responders.”
With his mission complete, the Grand Princess was allowed to dock and passengers to disembark from the ship. Those that showed symptoms of the virus had to be isolated and those that weren’t had to be quarantined — data now known thanks to Mr. Lovejoy and his team.
“And because of the nature of everything I ended up getting quarantined myself,” said Mr. Lovejoy, whose entire team spent 14 days at the University of Nebraska. “And fortunately we never ended up showing symptoms or getting sick.”
Both in quarantine and upon his return home and to work in late March, the lifelong Long Islander had a heightened fear, Dawn said, of contracting the novel virus.
“I have asthma, so I didn’t know how well I’d respond if I did get it,” Mr. Lovejoy added.
A quiet hero
When he left the Grand Princess March 9, there were 647 reported cases of COVID-19 in America, according to the Centers for Disease Control and Prevention (CDC). By the time he returned home March 23, there were more than 44,000 cases. That number nearly doubled when he returned to work a few days later.
Knowing this – and his particular risk — Mr. Lovejoy knew, still, where he needed to be. Like walking door-to-door on the Grand Princess, he floated from COVID unit-to-COVID unit at NSUH throughout the crisis, treating the explosion of patients showing up daily.
“When he went on the mission and when he goes to work every day, he knows how vulnerable he is,” Dawn said. “So, I consider him just a quiet hero, leading in his own way.”
Join the Northwell Health heroes keeping our patients and communities safe. Explore job opportunities.
Share this entry
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Subscribe to our blogs
Stay up to date with stories you want to know more about right to your email inbox.
Newsletter
Recent Posts
- Discover Kenneth’s career journey to a physical therapist at Northwell Health
- Explore two different career paths beginning as a nurse extern at Northwell Health.
- Mentorship, desired career growth, and making a difference: Meet Christopher, emergency department registered nurse
- Explore career paths in pharmacy at Northwell Health.
- From quality to operations: Discover Shivani’s career journey in labs
Categories
- Academia and Research
- Administrative Support
- Advance Clinical Providers
- Business
- Career Advice
- Career Paths
- Clinical Care
- Clinical Laboratory Science
- Clinical Support
- Culinary and Hospitality
- Culture
- EVS
- Featured Articles
- General Management
- Human Resources
- Imaging
- Inclusion and Belonging
- Information Technology
- Mentorship
- Nursing
- Operations
- Patient and Customer Experience
- Pharmacy
- Rehabilitation Services
- Revenue Cycle
- Social Services
- Students and Internships
- Veterans
- Wellness & Benefits
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
Archives
- May 2026
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
Contact us
If you are an individual with a disability requesting an accommodation for the application process, please click the contact us link above to request assistance.
Learn more about our hiring experience.
Read answers to common questions about the application process.
© 2026 - Northwell Health
If you are an individual with a disability requesting an accommodation for the application process, please click the contact us link above to request assistance.
Learn more about our hiring experience.
Read answers to common questions about the application process.
© 2026 - Northwell Health
It is Northwell Health’s policy to provide equal employment opportunity and treat all applicants and employees equally regardless of age, race, creed/religion, color, national origin, immigration status, or citizenship status, military or veteran status, sexual orientation, sex/gender, gender identity, gender expression, height, weight, disability, pregnancy, genetic information or genetic predisposition or carrier status, marital or familial status, partnership status, victim of domestic violence, their or their dependent’s sexual or other reproductive health decisions, or other characteristics protected by applicable law.
Northwell Health reserves the right to amend all terms of employment.


















